[Gynecological Laparoscopy] 4K Laparoscopic Uterine Perforation Repair
Release time: 07 Nov 2023 Author:Shrek
Uterine perforation is a serious gynecological complication. It is most common in surgeries that require intrauterine operations such as uterine curettage and hysteroscopy, but it is not limited to intrauterine operations. So, what are the culprits that cause uterine perforation? How to deal with uterine perforation?
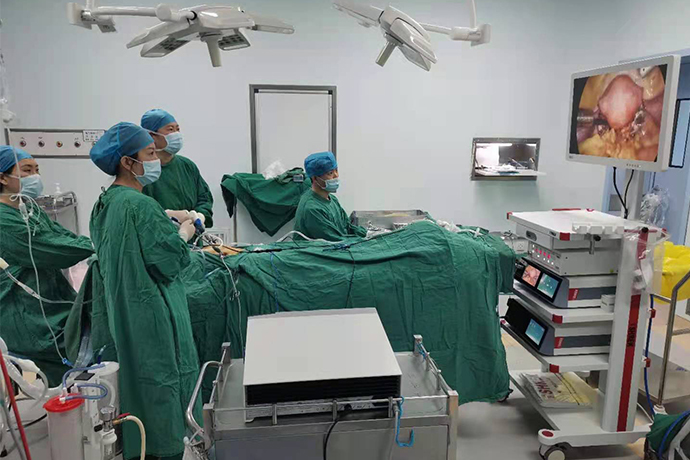
Causes of uterine perforation
1. Uterine factors: changes in the position of the uterus (excessive retroversion, close to the intestine), abnormal anatomical structures (such as uterine malformations, uterine fibroids, uterine cavity adhesions, etc.).
2. Cervical factors: Cervical stenosis, abnormal cervical structure (such as double uterus, single cervix) or scarring (such as caused by cone biopsy).
3. Vaginal factors: vaginal atrophy and stenosis during menopause.
4. Systemic factors: uterine softness during pregnancy, lactation, menopausal status, and long-term use of contraceptive pills; post-cesarean section, especially post-operative infections; cases of repeated artificial abortions or two artificial abortions that are very close together .
5. Operational factors: The size and position of the uterus were not clear before surgery; the surgical operation was not stable, accurate and light enough, and the operating procedures were not followed carefully. Or laparoscopic surgery to place a uterine cup, apply electrical instruments, etc.
6. There is malignant tumor in the uterus or reproductive tract.
Cervical dilation & curettage (suction)
Uterine dilatation and curettage or aspiration are one of the most common causes of uterine perforation, which often occur during induced abortion, uterine evacuation, and diagnosis and curettage. Perforation of the uterine cavity probe or uterine lift device may also occur when a uterine lift device is placed during laparoscopic surgery. .
History of previous uterine cavity operations, abortion or uterine evacuation during lactation, scarred uterus, excessive uterine flexion, uterine malformation (double uterus, septate uterus), molar evacuation are all high-risk factors for uterine perforation during uterine evacuation, and the diagnosis of long-term menopause Sexual dilation and curettage can also easily cause uterine perforation.
Hysteroscopic surgery
Among all complications of hysteroscopic surgery, the complication rate of uterine perforation is the highest, ranging from about 1% to 9%. Cervical stenosis and previous cervical surgery (cervical conization, laser treatment, etc.) may cause significant retroversion of the uterus. , perforation occurs due to retroflexion.
Postmenopausal atrophic uterus and excessive uterine expansion force, unclear intrauterine vision, excessive uterine expansion pressure, and lack of ultrasound monitoring during electroresection surgery are all risk factors for uterine perforation.
Intrauterine device insertion/removal
The most serious potential complication of IUD placement or removal is uterine perforation, with an incidence rate of 1/350 to 1/2500. Among them, 85% of perforations do not affect the normal function of other organs and have no clinical symptoms. 15% of perforations are possible. It can lead to serious complications such as rectal stenosis, rectal perforation, bladder fistula, and urethral fistula.
Common ones include complete uterine perforation involving the serosa layer and incomplete perforation in which the serosa layer remains intact, as well as complex uterine perforations involving adjacent intestines, greater omentum, etc. Uterine malformation, lactation, scarred uterine ring, and long interval between ring removal and menopause are all high-risk factors for IUD perforation.
Clinical manifestations of uterine perforation
The clinical manifestations of uterine perforation are related to the location and size of the perforation. When the surgeon is exploring the uterine cavity or performing uterine cavity operations, he suddenly feels a loss of uterine wall resistance and a bottomless feeling. The depth of the instrument entering the uterine cavity is far beyond the actual depth of the uterine cavity, and even adipose tissue or intestinal tubes are pinched out.
The patient suddenly feels pain in the lower abdomen. If the perforation involves large blood vessels, there will be symptoms of internal bleeding, such as pale complexion, profuse sweating, and drop in blood pressure. In severe cases, hemorrhagic shock may occur.
Depending on the perforation instrument, there can be different ultrasound manifestations.
1. If the probe is perforated, vaginal ultrasound will show thin strips of slightly higher echo in the muscle layer and discontinuous local echo in the serosa layer.
2. If the straw is perforated, abdominal ultrasound can show a pipe-like heterogeneous echo in the muscle layer at the perforation site, with the proximal end connected to the uterine cavity and the distal end penetrating the muscle layer.
How to deal with uterine perforation?
①The treatment of uterine perforation mainly depends on whether the perforation causes obvious intra-abdominal bleeding and damage to the intestines and other organs. Generally speaking, the operation should be stopped immediately when a perforation is discovered.
② If the vital signs are stable, the perforation site is far away from the uterine blood vessels or the perforation area is small, and there is no possibility of damage to the large blood vessels and intestinal tubes, close observation of the patient's vital signs, abdominal pain and vaginal bleeding, dynamic monitoring of hemoglobin changes and promotion of uterine contractions, Conservative treatment options to prevent infection.
③ For those with unstable vital signs or obvious signs and symptoms of abdominal pain and vaginal bleeding, or those with suspected uterine blood vessel damage causing broad ligament hematoma or intra-abdominal bleeding or the possibility of intestinal injury, laparoscopy or laparotomy should be performed to confirm the diagnosis and then stop the bleeding and remove the incarceration. Repair the perforation after tissue removal.
④ Pathological uterine perforation caused by malignant tumors or placental tissue erosion of the myometrium can be repaired after uterine artery embolization. If conservative surgery is not possible due to excessive bleeding, the uterus should be removed.
- Recommended news
- 【General Surgery Laparoscopy】Cholecystectomy
- Surgery Steps of Hysteroscopy for Intrauterine Adhesion
- [General Surgery Laparoscopy] 4K Ultra HD Laparoscopic Surgery for Acute Cholecystitis
- [General Surgery Laparoscopy] 4K ultra-high definition laparoscopic deroofing and decompression of renal cysts
- [Ureteroscopy in Urology] Laser lithotripsy for ureteral stones