[Gynecological Laparoscopy] 4K Laparoscopic Uterine Suspension Dubuisson Procedure
Release time: 01 Nov 2023 Author:Shrek
Uterine prolapse refers to the uterus descending from its normal position along the vagina, with the external cervical opening reaching below the level of the ischial spine, or even the entire uterus protruding outside the vaginal opening, often accompanied by bulging of the anterior and/or posterior vaginal walls. The front and back walls of the vagina are adjacent to the bladder and rectum, so uterine prolapse can also be accompanied by vesicourethral and rectal bulges. Uterine prolapse is related to the relaxation of the ligaments that support the uterus and the weakening of the pelvic floor support. Common causes include:
1: Childbirth injuries
It is the main cause of uterine prolapse.
2: Increased abdominal pressure
Chronic constipation and cough, ascites or abdominal obesity can increase abdominal pressure and promote uterine prolapse.
3: Congenital developmental abnormalities
Uterine prolapse in nulliparous women is caused by underdevelopment of reproductive organ support tissues.
4: Malnutrition
Severe nutritional deficiencies can lead to muscle atrophy, pelvic fascia relaxation, and loss of support for the uterus.
5: Aging
Hypoovarian function leads to a decrease in estrogen secretion, which makes the supporting tissue of the pelvic floor weak and loose, prone to prolapse, or aggravating the original degree of prolapse.
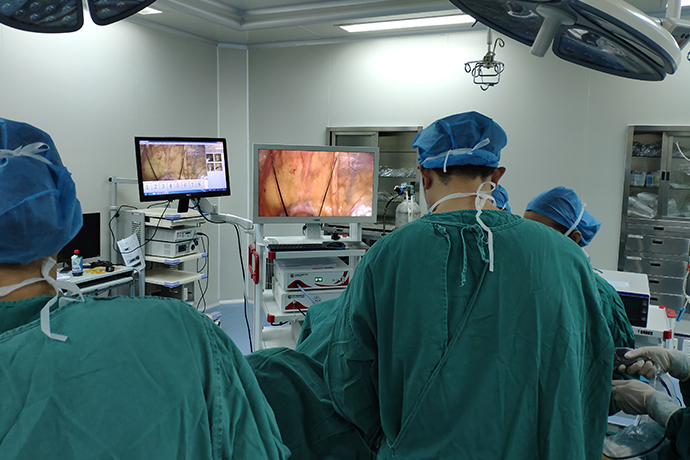
Patients with uterine prolapse often feel that their abdomen drops and their backs are sore, which is more obvious when walking and squatting. In patients with mild prolapse, vaginal prolapses can be retracted by themselves after lying down and resting. Conservative treatment is often recommended, avoiding abdominal pressure activities, keeping stools unobstructed, reducing standing time, and actively exercising pelvic floor muscles. For moderate and severe patients, the prolapse cannot be restored, and the mucosal surface of the cervix may thicken, become keratinized, or suffer from erosion and ulceration due to long-term exposure. Patients have increased leucorrhea, sometimes pus-like or bloody, and some have menstrual disorders and excessive menstrual bleeding. When accompanied by cystocele, difficulty in urinating, urinary retention, stress urinary incontinence, etc. may occur, seriously affecting the patient's life. At this time, surgical treatment needs to be considered. In the past, the conventional surgical treatment for patients with uterine prolapse was total abdominal or transvaginal hysterectomy + vaginal repair, but the postoperative recurrence rate was as high as 30%-40%. In recent years, laparoscopic technology has been widely used in clinical practice depending on the age and condition of the patient.
Common treatments
Mild patients with POP-Q I-II degrees without conscious symptoms can improve their lifestyle (weight loss, quit smoking, reduce activities that increase pelvic floor pressure, treat constipation and cough, etc.), pelvic floor muscle exercises (Kegal training), pelvic Rehabilitation therapy (electrical stimulation, biofeedback, magnetic therapy, etc.), pessaries, traditional Chinese medicine, acupuncture and other non-surgical treatments.
Symptomatic patients with POP-Q II degree or above have better recovery outcomes through surgical treatment. There are two main types of surgeries for POP:
1. Traditional surgeries, including anterior and posterior vaginal wall repair, vaginal hysterectomy, vaginal closure, etc. Traditional hysterectomy + anterior vaginal wall repair will weaken the supporting strength of the pelvic floor tissue after hysterectomy, which will cause prolapse of the vaginal stump, increase the recurrence rate and the risk of secondary surgery; and sexual life cannot be carried out after vaginal closure, It is not suitable for young patients and patients who still need sexual life, so the above-mentioned surgery is currently relatively rarely used in clinical practice.
2. Pelvic floor reconstruction using autologous tissue or mesh. It can be performed transvaginally, transabdominally, or laparoscopically. This procedure is not only beneficial to restoring the normal anatomical position of prolapsed organs, but the supporting role of the mesh can also restore the function of prolapsed organs, relieve uncomfortable symptoms, and has good clinical effects.
Among them, Laproscopic lateral suspension (LLS) uses mesh to restore the uterine/vaginal stump to its normal position and suspend it on the lateral abdominal wall to prevent recurrence. It is currently widely used in clinical practice. The surgery can be performed with or without preserving the uterus, and is especially suitable for the treatment of pelvic organ prolapse in young women and overweight women who have frequent sexual intercourse.
Laparoscopic lateral abdominal wall suspension
Laproscopic lateral suspension (LLS), also known as Dubuisson surgery, is a new technology that replaces sacral fixation. This surgery has been used to treat POP for ten years in Europe.
LLS uses two meshes sneaking outside the peritoneum on the left and right sides to simulate the point of force of the round ligament in the uterus. Through the friction between the transverse mesh and the anterior abdominal wall tissue, the top of the uterus or vagina is lifted and suspended in the pelvic cavity. . The mesh only needs to be simply passed through the peritoneum, without the need to nail the mesh to the sacrum and any ligamentous structures, avoiding periostitis, reducing postoperative pain, reducing the risk of irritation and damage to the hypogastric plexus, and avoiding the sacral promontory area, including the iliac blood vessels. , aorta, vena cava, ureter and rectum injuries.
LLS has good surgical results mainly for anterior pelvic prolapse with or without partial mid-pelvic prolapse. Compared with pelvic floor reconstruction surgery with transvaginal mesh, LLS also reduces the risk of mesh exposure and erosion, reduces the risk of organ damage and bleeding during puncture, is less difficult to learn, and is more suitable for a wide range of clinical applications. promotion.
Advantages of LLS surgery
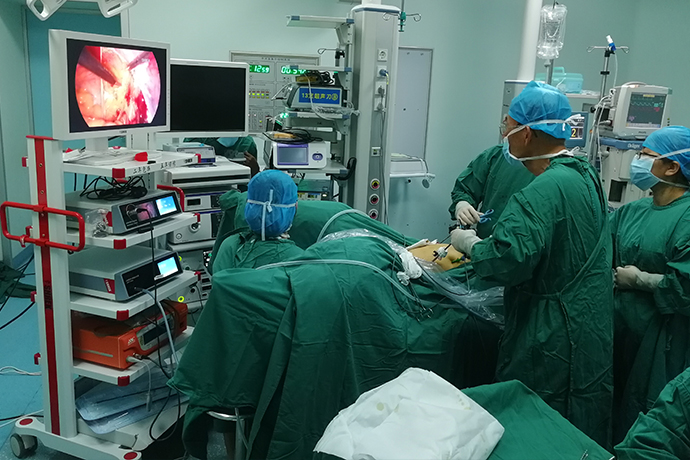
Minimally invasive: 4K laparoscopy is performed under direct viewing through a large display screen, avoiding blind punctures. The surgical field of view is clearly visible, which is convenient for doctors to operate. It has higher accuracy, minimally invasive surgery and fast healing.
High safety: The surgical path is clearly visible and easily avoids the easily damaged ureter, hypogastric nerve plexus, presacral venous plexus and intervertebral disc. The surgical risk is small, there is less bleeding, the operation time is short, the postoperative recovery is fast, and there are no postoperative complications. few.
High effectiveness: The success rate of anatomical reduction is high, symptoms are significantly improved, and the recurrence rate is low; it can maintain the normal axis of the uterus, the integrity of the pelvic floor tissue, and the normal vaginal length, allowing the patient and his spouse to enjoy a higher quality of life after surgery. quality.
Surgical steps:
1. The patient is placed in the supine bladder lithotomy position, under general anesthesia and sterilized draping.
2. First of all, patients with vaginal front and back wall bulge should undergo routine vaginal wall repair, and patients with long cervix should undergo partial cervical resection. Otherwise, once the prolapsed uterus is suspended and fixed to the anterior abdominal wall, vaginal surgery can be performed. Operation will be more difficult.
3. Our long-term follow-up shows that this surgery cannot improve tension urinary incontinence. It is recommended that patients with tension urinary incontinence be treated with corresponding surgeries such as TVT or TVT-O.
(1) Suspension fixation of the anterior abdominal wall of the uterus using the round ligament method:
For young patients with uterine prolapse or even those with potential fertility requirements, if the round ligament is relatively tough, we can use round ligament traction and suspension to fix the uterus to the anterior abdominal wall.
1. Cauterization of the serosa layer of the anterior uterine wall: Use electrosurgical instruments to cauterize the serosa layer of the anterior uterine wall to form dense adhesions between the anterior uterine wall and the anterior abdominal wall after surgery. Note that the burning surface should not exceed the reflex of the bladder, uterus, and peritoneum to avoid damaging the bladder. The corresponding anterior abdominal wall peritoneum does not need to be cauterized.
2. Determination of the suspension position of the anterior abdominal wall: The assistant pushes the uterus upward from the vagina to the normal position. The surgeon uses his fingers to gently press the anterior abdominal wall on the midline of the umbilical pubic abdomen, and evaluates and selects the appropriate position of the suspension incision under direct vision of the laparoscope. Our experience is that the bottom of the uterus corresponds to the anterior abdominal wall, which is generally 1-5cm above the upper edge of the pubic symphysis, depending on the size of the uterus.
3. Puncture method of the anterior abdominal wall at the suspended part: Select a good location on the umbilical pubic line, make a 5mm incision on the skin of the anterior abdominal wall, insert a 5mm puncture device vertically into the skin and subcutaneous, and when the first Stop puncture when a resistance point occurs. This resistance point indicates that the puncture tool has reached the surface of the anterior sheath of the rectus abdominis muscle. At this time, slide the puncture device 2-3cm to the left side along the surface of the rectus abdominis muscle, and then insert it into the abdominal cavity under direct vision of the laparoscope.
4. Clamp the round ligament: Insert a 5mm laparoscopic Alice forceps (Allis grasper) into the abdominal cavity along the trocar cannula, and clamp the left round ligament about 1cm away from the uterine angle. Do not clamp the tip of the forceps. Hold the round ligament to avoid damaging the round ligament.
5. Pull the round ligament on one side to the outside of the abdominal wall: close the inlet valve of the puncture cannula, open the outlet valve, release part of the intra-abdominal CO2, and appropriately reduce the intra-abdominal pressure while maintaining a clear field of vision. Then drag the left round ligament and the puncture cannula out of the body along the puncture tunnel in the abdominal wall, and use a pair of Alice forceps for laparotomy to fix the round ligament.
6. Pull the round ligament on the other side to the outside of the abdominal wall: re-inflate the pneumoperitoneum, insert the 5mm puncture vertically along the original incision again, stop puncture when it reaches the surface of the anterior sheath of the rectus abdominis, and slide 2-3cm to the right side , then penetrate the abdominal cavity under direct vision of the laparoscope, and pull the right round ligament out of the body in the same way as the left round ligament.
7. Suture the round ligaments on both sides outside the abdominal wall: Use thicker non-absorbable sutures to suture and tie the round ligaments on both sides. The surface of the round ligament can be cauterized outside the body before suturing, in order to prevent adhesion between the left and right round ligaments as well as between the round ligament and the tissue surrounding the abdominal wall tunnel after surgery.
8.Check the suspension effect: Inflate the pneumoperitoneum and check carefully to ensure that the anterior wall of the uterus can be in close contact with the anterior abdominal wall after the suspension is fixed. It is important not to separate the anterior wall of the uterus from the anterior abdominal wall, forming a "swing"-like suspension. The round ligament has limited toughness and cannot resist gravity and abdominal pressure alone. In this operation, the round ligament plays a temporary fixation role, relying on the adhesions formed after the operation to fix the tough tissue of the uterus as a pulling object on the tougher rectus abdominis muscle and the anterior sheath of the rectus abdominis muscle to resist gravity and abdominal pain. Press 1. Once a "swing"-like suspension is found, it indicates that the part where the round ligament is lifted by the forceps is too far from the uterine angle. The thread knot on the surface of the subcutaneous anterior rectus abdominis sheath should be cut and a suitable position should be re-selected along the round ligament toward the uterine angle. The lifted area is lifted and sutured again to fix it.
If it is found that the round ligament has been damaged during the above operation and is too weak, and it is estimated that it will be difficult to maintain traction and fixation of the uterus, then the suture-based suspension fixation procedure we will introduce later will need to be performed, but the patient should be informed of the suture-based suspension fixation procedure. The method will not be able to complete childbirth, and the patient may need sterilization during the operation or should take contraceptive measures after the operation.
(2) Suture fixation of the anterior abdominal wall of the uterus
For older women or women who have no desire to have children, sutures may be used to suspend the uterus to the anterior abdominal wall. In our practice, the vast majority of patients adopt this surgical method and the results are satisfactory.
1. Cauterize the serosal surface of the anterior wall of the uterus
2. Suture through the uterus: use a large circular needle (use the largest possible circular needle) and non-absorbable suture (such as double-stranded No. 10 silk thread or the polyester non-absorbable suture used to suture tendons in orthopedics), on the right side of the uterus from front to back The uterus is sutured through the back, and then the uterus is sutured through the uterus from back to front on the left side of the uterus. Note that during the above suturing process, try to avoid the suture passing through the uterine cavity. Remove the needle and keep the suture.
3. Pull the penetrating uterine suture to the outside of the abdominal wall: As mentioned above, make a 5mm skin incision at an appropriate position on the midline of the umbilical pubic abdomen, insert the 5mm puncture device, and stop the insertion at the first resistance point , slide 2-3cm sideways on the surface of the anterior rectus abdominis sheath, and continue to insert the puncture device into the abdominal cavity. Clamp the end of the suture on one side and pull it out of the body together with the puncture device for later use. In the same way, pull the tail end of the suture on the other side out of the body.
4. In vitro knotting of penetrating uterine sutures: Tighten the sutures in vitro, and tie the left and right sutures into a knot on the surface of the rectus abdominis muscle. If necessary, you can use a knot pusher to push the knot to the rectus abdominis muscle. Anterior sheath surface. To prevent slippage, it is recommended to tie at least 3 knots.
5.The method of checking the postoperative effect is the same as that of round ligament suspension.
Different from the round ligament method, once patients of childbearing age become pregnant after using this method to correct uterine prolapse, the sutures used to fix the uterus cannot extend with pregnancy like the round ligament. Therefore, sterilization can be considered during the operation for patients of childbearing age. Surgery 2.
- Recommended news
- 【General Surgery Laparoscopy】Cholecystectomy
- Surgery Steps of Hysteroscopy for Intrauterine Adhesion
- [General Surgery Laparoscopy] 4K Ultra HD Laparoscopic Surgery for Acute Cholecystitis
- [General Surgery Laparoscopy] 4K ultra-high definition laparoscopic deroofing and decompression of renal cysts
- [Ureteroscopy in Urology] Laser lithotripsy for ureteral stones