[Thoracoscopic Thoracic Surgery] 4K ultra-high definition thoracoscopic lobectomy
Release time: 14 Nov 2023 Author:Shrek
For some people with lung disease, doctors may recommend a lobectomy.
The preferred treatment for early-stage lung cancer is surgery, which inevitably leads to trauma. Traditional thoracotomy surgery has large incisions, severe trauma, slow postoperative recovery, and some patients even suffer from postoperative dysfunction. In order to reduce surgical trauma, surgeons are constantly making various attempts and explorations. It was not until the early 1990s that the application of endoscopic technology in lung cancer surgery significantly reduced surgical trauma. The endoscope is inserted into the chest, and the scene in the chest is truly broadcast to the display screen through the imaging system. The doctor only needs to make 3 to 4 small holes in the patient's body, and use special surgical instruments to scan the images on the display screen. The operation can be completed, which is video-assisted thoracic surgery (VATS). With the advancement of technology, in addition to multi-hole VATS, double-hole video-assisted thoracoscopic lung cancer minimally invasive surgery (single-operating hole minimally invasive lung cancer surgery) has gradually become popular in clinical practice: two holes are drilled in the human body, one with a diameter of about 1cm, and a After placing the video thoracoscope, the other hole is about 3 cm long, which is used for the entry and exit of surgical instruments, and the diseased lung tissue is removed through this hole.
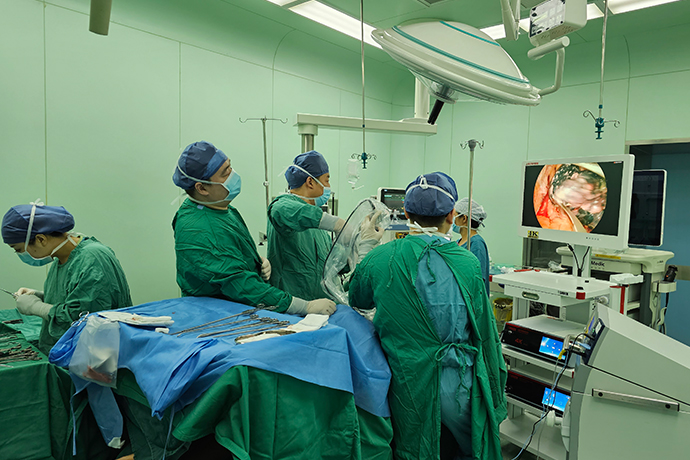
Since the first lobectomy using single-port video-assisted thoracoscopic surgery (uVATS) in 2010, the use of this technology has continued to expand around the world. Compared to the multiport approach, single port offers a range of benefits such as direct view, better lung exposure, ergonomic instrumentation, less postoperative pain, faster postoperative recovery, shorter hospital stay, and Helps implement adjuvant treatment earlier.
Incision location:
The general rule of thumb for any lobectomy is to choose an incision in the 5th intercostal space between the mid-axillary and anterior axillary lines. This position allows the surgeon to approach the hilum at a slight angle, allowing hand instruments to be manipulated along the longitudinal axis. When the incision is too high, the surgical axis is too close to the hilum. Although the anatomy is not an issue, the lack of angle means that the hand instrument cannot bypass the blood vessels and is instead pushed against the posterior hilar structures. If the incision is too low, the shaft provides a good angle for the stapler, but the incision is far away from the hilum and the instrument operation path is very narrow, complicating instrument operation (Figure 3). When performing upper lobectomies (right upper lobectomy for right-handed surgeons, left upper lobectomy for left-handed surgeons) and central lesions for which sleeve resection is possible, the use of the fourth intercostal space is recommended because it allows for more Well exposed and handled.
Ideal position: The incision in the fifth intercostal space allows the surgeon to access the portal at a slight angle, allowing hand instruments to be manipulated along the longitudinal axis. The incision position is too high: When the incision is too high, the operating shaft directly enters the hilum. While the anatomy is not an issue, the lack of angle means that the hand instrument cannot bypass the blood vessels and is instead pushed against the posterior hilar structures. The incision is too low: If the incision is too low, the shaft provides a good angle for the stapler, but the incision is far away from the hilum and the instrument operation path is very narrow, making instrument operation complicated.
The anterior incision position naturally provides maximum opening of the intercostal space, allowing the use of more ergonomic instruments and reducing postoperative pain. When operating on the left side, the incision should be slightly lateral to minimize interference with the beating of the heart. The size of the incision depends on the surgeon's experience, but is usually 3-4 cm long. During the learning process, it cannot be too big (no more than 6 cm, because the lens and instrument lose support points) or too small (no less than 3 cm, to avoid too small space between the lens and instrument). The incision adopts a muscle-sparing technique: the serratus anterior muscle is opened without cutting its fibers, the intercostal muscles are separated from the upper edge of the lower ribs, and the intercostal pedicles are preserved. In order to prevent postoperative subcutaneous emphysema, the intercostal space should not be expanded.
In obese patients and sleeve resections, the use of a wound protector can be convenient to prevent tumor recurrence and is highly recommended during the learning curve. Lubricant applied to the outside facilitates entry of the lens and instrument and reduces friction between them. The medial side may limit the angle of the instrument, so in the case of chest wall adhesions it is best to loosen the part closest to the incision before inserting the protective sheath. In the absence of a wound protector, the soft tissue on both sides can be sewn on the surgical drape to pull the soft tissue and keep the incision open, otherwise intrathoracic suction will inflate the lungs and hinder the operation. If the wound or its surroundings are not completely bloodless due to nearby adhesions, it is also helpful to place gauze between the lens and the incision to prevent blood from dripping onto the lens.
All specimens must be removed using a retrieval bag without touching the edges of the incision. For small specimens like lymph nodes, surgical gloves are a cost-effective alternative. To remove large specimens, Sihoe et al described a simple technique of incising 1 rib anteriorly to open the intercostal space and avoid the use of a rib expander. A simple figure-of-eight suture is enough to stabilize the ribs. After the surgery, a chest drain is placed through a single port, usually at the back of the incision. Careful closure is recommended to avoid interlaminar gaps and to prevent subcutaneous emphysema along the pleural duct.
How do doctors make the decision that lobectomy is the best lung cancer surgery for a patient? Doctors recommend several factors to consider when performing lung cancer surgery:
1. The location of the tumor
2. Tumor size
3. Whether the swelling invades adjacent tissues
4. Patient’s general health
5. Preoperative lung function
The human lungs are composed of five lobes. There are three slices in the right lung and two slices in the left lung. A lobectomy removes one of the lungs. After surgery, the healthy lung lobes will compensate for the function of the removed lung lobes, and the lung function can maintain the preoperative state, or even be better than before the surgery.
Lobectomy is suitable for other single lobe diseases, such as:
1. Tuberculosis
2. Emphysema
3. Benign tumors
4. Fungal infection
5. Lung abscess, that is, purulent lesions of lung tissue
After the diseased lung lobe is removed, the other lung lobes will automatically expand to help the patient breathe more smoothly.
Preoperative preparation
Sterile dressings: dressing, surgical gown, three sheets, large bowl, cavity base, thoracoscope, 30° lens, endoscopic gauze, 1 round head of electrosurgery, medium leather, iron suction head, lamp handle, incision protection , disposable puncture sheath, 1.4.7 mousse thread.
Disposable items: indwelling needle, intravenous patch 3, incision patch small 4 medium 2, cerebral membrane, red urinary catheter, catheter bag, biling 2, chest closed drainage tube 2, water seal bottle 2, protective cover 2. Imported titanium clip, body temperature probe, cutting and closing device, double-lumen tube, deep penetration bag, pressure sensor, puncture needle, tee 3, extension tube 3.
Cooperation with surgery
1. Disinfect the skin first, hand over the surgical film, and use a piece of dry gauze to assist in applying the film.
2. Prepare thoracoscope items, connect, check and adjust the thoracoscope camera system and surgical instruments.
3. Use the blade to cut the skin and make holes.
1. Treatment of pleura and fissures
Separation of adhesions: Oval forceps pull the lung tissue to provide a certain tension, and the interface is the fat layer that is seen during separation; an ultrasonic scalpel can also be used to separate.
Separation of pulmonary fissure (horizontal fissure): The endoscopic cutting and dividing device cuts the lung tissue, separates the tunnel between the middle and upper lobe branches of the superior pulmonary vein, and the endoscopic cutting and dividing device is used for incision and the titanium clip is used before releasing the lower pulmonary ligament. Clamp or ligate with No. 7 wire, and then use an electrocoagulation hook to incise the inferior pulmonary ligament.
2. Vascular treatment
The inferior pulmonary vein is freed and disconnected.
The branches of the pulmonary artery are ligated or sutured or clamped with silk thread.
3.Bronchial treatment
Free bronchus; disconnect bronchus.
Surgery completed
Cooperation with surgery
1. Specimen removal: After cutting out the lung lobes, use oval forceps to clamp the bronchial stump as a pulling point.
2. Thoroughly stop bleeding in the chest. After flushing, ask an anesthetist to assist in inflating the lungs. Check that there is no air leakage and the lower lobes are fully inflated. After the lungs are inflated, a chest drainage tube is placed and fixed. Remove the thoracoscope and instruments, inventory the items, and close the incision layer by layer.
3. The circulating nurse connects the water-sealed bottle off the stage, pours 500ml of saline into the chest bottle, and writes it with tape and sticks it on the scale. Mark the drainage tubes well.
4. Suture and cover the incision, hand forceps with teeth, hold the large circular needle No. 7 thread with the needle holder to suture the subcutaneous layers, suture the skin with a triangular needle, disinfect the incision skin with iodophor cotton balls, cover it with a dressing, and connect the water seal bottle.
- Recommended news
- 【General Surgery Laparoscopy】Cholecystectomy
- Surgery Steps of Hysteroscopy for Intrauterine Adhesion
- [General Surgery Laparoscopy] 4K ultra-high definition laparoscopic deroofing and decompression of renal cysts
- [Ureteroscopy in Urology] Laser lithotripsy for ureteral stones
- [Laparoscopic Urology] Laparoscopic Radical Right Nephrectomy