【Gynecological Hysteroscopy】Myomectomy
Release time: 16 Aug 2022 Author:Shrek
Uterine fibroids are a disease with a high incidence of women, which brings great distress to patients physically and psychologically: menstrual disorders, heavy menstrual flow, infertility, and psychological fear even if there are no symptoms. The emergence of hysteroscopic resection of uterine fibroids has opened up a new way for the treatment of uterine fibroids in a minimally invasive way.
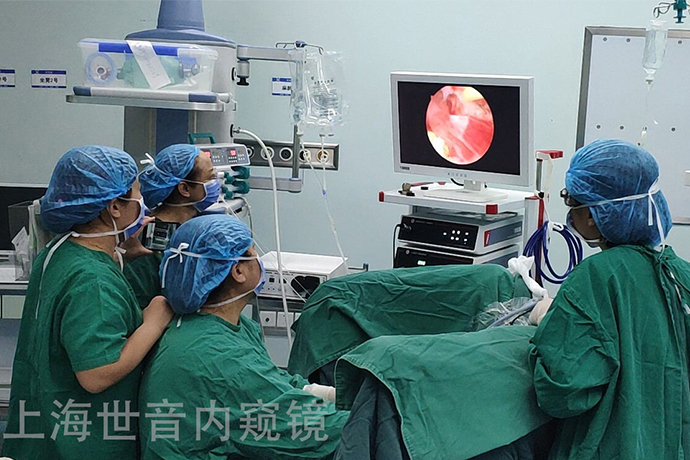
Hysteroscopic myomectomy is the use of hysteroscopic techniques to enter the uterine cavity from the cervix through the vagina and remove the submucosal fibroids under the hysteroscope.
Uterine fibroids are classified according to where the uterus is located. Submucosal fibroids are associated with abnormal uterine bleeding. When these fibroids show symptoms, they should be surgically removed, and the method of removal depends on the type of fibroids.
The classification of uterine fibroids has a guiding role in clinical treatment. According to the traditional classification of uterine fibroids, they are divided into uterine fibroids and cervical fibroids. According to the different parts of fibroids in the uterine muscle wall, they are divided into 3 categories: intramural fibroids, subserosal fibroids and mucosal fibroids. lower fibroids. However, with the development of hysteroscopic laparoscopy, traditional classification is difficult to meet clinical needs, and the classification of uterine fibroids tends to be refined. The most commonly used method is the FIGO classification of uterine fibroids.
Corresponding to the FIGO classification of uterine fibroids, there are three types of submucosal fibroids (FIGO 2010):
①Type 0, pedunculated submucosal uterine fibroids
②Type 1, the fibroids protrude to the uterine cavity > 50%
③Type 2, fibroids protruding to the uterine cavity ≤ 50%.
There are two types of intramural fibroids (FIGO 2010):
①Type 3, intramural fibroids in contact with the endometrium
②Type 4: Complete intramural uterine fibroids.
Subserosal fibroids include three types (FIGO 2010):
①Type 5: The fibroids are convex toward the serosa, and the convexity is less than or equal to 50%
②Type 6: fibroids protrude toward the serosa, convex > 50%;
③Type 7: pedicled subserosal fibroids.
In addition, type 8 are other types (special sites such as cervix, broad ligament fibroids), and miscellaneous uterine fibroids are fibroids embedded between the endometrium and serosa.
The development of myomectomy
In 1978, Neuwirth performed the first hysteroscopic myomectomy using a urinary resectoscope, a surgical technique similar to a prostatectomy, using a direct-view resectoscope and a "U" ring to cut the fibroids into thin slices, But sometimes the adjacent myometrium is damaged. Myomectomy, also known as the "gold standard" technique, can lead to severe exposure of the vascular mass, which can cause excessive bleeding, excessive fluid absorption, and sometimes damage to the myometrium, which can affect fertility.
Some doctors have performed pseudocapsule-sparing hysteroscopic myomectomy. Litta et al loosened a portion of the intrauterine fibroids after excision, while Mazzon used a cold knife to loosen the intramural fibroids. This technique, published in Brazil in 2002, is similar to open or laparoscopic myomectomy to preserve the pseudocapsule. Instead of partial resection, the entire fibroid is loosened. Considering the integrity of the pseudocapsule is more conducive to the operation. .
This technique uses a resectoscope (Collins) with an "L" ring, first completely encircling the tumor bed, thereby accessing the fibroid interface/pseudocapsule, loosening fibrous bundles, and occasionally finding clotted vessels. There is generally a vascular network surrounding the fibroids, and fibroids dissection within the pseudocapsule will reduce bleeding and preserve the integrity of the myometrium, thereby promoting uterine healing and benefiting future reproductive outcomes.
Management of uterine fibroids
Since most patients with uterine fibroids are asymptomatic, observation and follow-up are often used. Drug therapy is mainly for patients who are temporarily unable to operate and need to improve symptoms, such as anemia. Surgical treatment includes myomectomy and hysterectomy, which are selected according to the patient's age, condition and needs. Surgical approaches include laparotomy, laparoscopy, hysteroscopy and vagina. Non-surgical treatments include uterine artery embolization and high-intensity focused ultrasound therapy.
Hysteroscopic myomectomy
(1) Indications of TCRM
The indications for hysteroscopic resection of uterine fibroids are: ① FIGO type 0, 1, 2 and some patients with type 3 (the fibroids are close to the endometrium and have fertility preservation needs); ② The size of the fibroids is generally ≤5cm, The size of the fibroids protruding from the vagina is not limited; ③ Those with clinical symptoms, such as abnormal uterine bleeding or fertility requirements; ④ Exclude endometrial lesions; ⑤ The size of the uterus is generally limited to within 10 weeks of pregnancy, and the depth of the uterine cavity is <12cm; Uterine fibroids were excluded.
(2) Preoperative preparation for TCRM
1. General preparation and special preparation
Like other surgeries, a series of preoperative examinations and evaluations such as chest X-ray, electrocardiogram, blood routine, and coagulation are required before TCRM surgery. In addition, the following special preparations are required before TCRM surgery.
1)Uterine fibroids pretreatment
Use diagnostic hysteroscopy to examine the cervical canal and uterine cavity to understand the location of uterine fibroids, their relationship with the uterine wall (that is, what type of fibroids), their size, and whether there are other combined lesions in the uterine cavity. After hysteroscopy confirmed the diagnosis, the hysteroscope was withdrawn.
Exploration of the uterus and dilation of the cervical canal (usually dilated to size 10, depending on the outer diameter of the resectoscope used).
A hysteroscope with ring electrodes was placed under direct vision.
Under the hysteroscope, the fibroids were passively removed one by one from the surface of the fibroids with a ring electrode until the fibroids were completely removed. During the excision, attention should be paid to distinguish the layers of fibroids and the uterine wall under the microscope. Do not remove too deep and remove the myometrium, or even the possibility of uterine perforation; and no residual fibroids.
It was observed under hysteroscopy that after the fibroids had been removed, there were no ejection bleeding points, and the hysteroscopic body was withdrawn. Observe the uterine bleeding. If there is no obvious bleeding, end the operation; if there is obvious bleeding, analyze the cause and treat it symptomatically (such as promoting uterine contractions, coagulating bleeding arteries under hysteroscopy, etc.)
(3) Surgical skills
1. Hysteroscopic surgical treatment of type 0 submucosal uterine fibroids: First, the fibroids that can be completely removed through the cervix can be removed with a ring electrode after removing the root of the fibroids and then holding them with oval forceps. Second, for those with larger fibroids, it is necessary to cut the fibroids anterogradely from both sides of the fibroids with a ring electrode, and cut the fibroids into "grooves". Pay attention to the contralateral endometrium during the cutting process. Then use oval forceps to hold and twist to remove, trim the tumor cavity and stop bleeding as appropriate. Third, for the fibroids that protrude into the vagina, the fibroids are cut off under the hysteroscope.
2. Hysteroscopic surgical treatment of type 1 and type 2 submucosal fibroids Because most of type 1 uterine fibroids are located in the uterine cavity, the same treatment as type 0 is required, but attention should be paid to endometrial protection for those who have fertility requirements. In type 2 uterine fibroids surgery, the electrode is used to cut the tumor capsule at the most prominent part of the fibroids, so that the fibroids protrude into the uterine cavity, and then remove them. When the fibroids are large, oval forceps can also be used to clamp them. Removal; intraoperative use of pituitary hormone, oxytocin, water separation and other methods to promote the movement of fibroids into the uterine cavity. For fibroids that cannot protrude into the uterine cavity, it is not advisable to forcibly dig into the muscle wall, and the fibroids should be excised until they are parallel to the surrounding muscle wall. The remaining part of the fibroids should undergo a second operation depending on the postoperative growth, or under ultrasound monitoring. Surgery to reduce the occurrence of uterine perforation. For multiple uterine fibroids, the larger fibroids are usually removed first to make the surgical field clear. During the procedure, try not to damage the pseudocapsule.
Due to the high requirements of hysteroscopic surgery for type 2 uterine fibroids, sometimes a second operation is required. You can refer to the following table for preoperative evaluation.
3. Hysteroscopic surgical management of type 3 submucosal uterine fibroids
It is mainly implemented for patients with infertility or recurrent miscarriage without other abnormal causes. Under the supervision of B-ultrasound, the needle electrode cuts the mucosa on the surface of the fibroids, and then withdraws the scope, uses oxytocin to promote the fibroids to the uterine cavity, and then removes them. Fractional surgery.
4. Hysteroscopic surgical management of cervical fibroids
A ring electrode was placed slightly below the junction between the cervical fibroids and the cervical canal, and the pedicle was partially cut by electric incision to make it thinner and cut off. Finally, the oval forceps were used to twist it out.
5. Monitoring of submucosal uterine fibroids during hysteroscopic surgery
Intraoperative ultrasound monitoring can observe the size, number and location of fibroids, especially the depth of fibroids involved in the myometrium. It can also observe the boundary between the uterine wall and surrounding myometrium of uterine fibroids, and measure the distance between the outer edge of fibroids and the serosa. , which can not only assist in the complete removal of fibroids, but also prevent uterine perforation, especially in large fibroids surgery. Ultrasound has a monitoring and guiding role.
Intraoperative laparoscopic monitoring is mainly used for larger submucosal uterine fibroids, especially those with deformed uterine cavity. Laparoscopic monitoring can detect uterine perforation and incomplete perforation in time, and suture it immediately.
6. Management of intraoperative bleeding
If it is intraoperative bleeding that has not been completed, hysteroscopic electrocoagulation to stop bleeding, application of uterine contraction drugs, and increased perfusion pressure can be used to stop bleeding. After uterine perforation was ruled out, the operation was stopped and the bleeding was stopped by compression with a Foley ureteral balloon. If the operation has been completed, the bleeding can be stopped by direct pressure with the Foley ureteral balloon. When the Foley ureteral balloon is used to compress the hemostasis, the balloon is filled with water until there is no obvious bleeding in the cervical canal, and then it is removed 6-8 hours after the operation.
7. Intraoperative precautions
Intraoperative attention should be paid to the protection of the endometrium, especially for multiple uterine fibroids, to reduce the chance of postoperative adhesions. For large uterine fibroids, if it is considered that they cannot be removed at one time, operations can be performed in stages to reduce the occurrence of complications. If necessary, blood gas can be checked during the operation, and furosemide can be administered intravenously to prevent hyponatremia. The operation time should not exceed 1 hour as much as possible, and the pressure of uterine distention should not exceed 100mmHg to reduce the occurrence of water intoxication. Postoperatively, the pressure of uterine dilatation should be reduced. For fluctuating bleeding, electrocoagulation should be used to stop bleeding in time to reduce the chance of postoperative bleeding.
8. Postoperative Management
For patients with fertility requirements and larger wounds, estrogen therapy can be given after surgery to promote endometrial growth, accelerate epithelialization, and prevent adhesions. The use of estrogen needs to fully evaluate whether the patient has contraindications, especially for patients with multiple uterine fibroids, the size of the residual fibroids is also a factor to be considered, and the patient should be fully communicated before use. Hyaluronic acid can also be placed postoperatively to prevent adhesions. For patients with a lot of postoperative bleeding, oxytocin is used after surgery. When the effect is not good, Foley ureteral balloon can also be used to stop the bleeding.
Summarize
Hysteroscopic myomectomy (TCRM) is less traumatic and less bleeding, especially for the treatment of uterine submucosal fibroids, without destroying the anatomical structure of the uterine muscle wall, and the postoperative recovery is fast. For those who need fertility, it can also shorten the operation It is known as the standard surgical method for the treatment of uterine submucosal fibroids. However, caution must be exercised when performing hysteroscopic resection. Before surgery, the necessity of hysteroscopic resection and the risks of surgery should be fully assessed, preoperative preparations should be made, surgical skills should be improved, and surgical skills and corresponding post-operative treatment methods should be mastered. Endometrial, preventing postoperative adhesions and reducing surgical complications.
- Recommended news
- 【General Surgery Laparoscopy】Cholecystectomy
- Surgery Steps of Hysteroscopy for Intrauterine Adhesion
- [General Surgery Laparoscopy] 4K ultra-high definition laparoscopic hiatal hernia repair
- [General Surgery Laparoscopy] 4K Ultra HD Laparoscopic Surgery for Acute Cholecystitis
- [General Surgery Laparoscopy] 4K ultra-high definition laparoscopic deroofing and decompression of renal cysts