【Laparoscopy】Hepatobiliary and pancreatic surgery
Release time: 11 May 2022 Author:Shrek
Compared with traditional open surgery, laparoscopic surgery has the advantages of less trauma, less systemic reaction, less intraoperative bleeding, shorter hospital stay, lower morbidity and better cosmetic results. More and more minimally invasive techniques represented by laparoscopic surgery are gradually replacing traditional surgical operations.
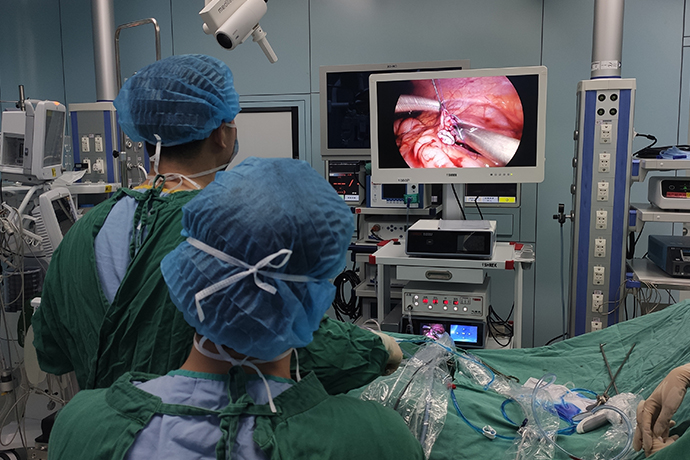
Hepatobiliary and pancreatic surgery is the most complex and traumatic surgical area in abdominal surgery, and laparoscopic hepatobiliary and pancreatic surgery is difficult to operate. However, after more than 20 years of clinical practice, laparoscopic liver surgery is safe and effective for surgeons with rich experience in hepatobiliary surgery and laparoscopic surgery.
Surgical Equipment & Instruments
1. Equipment: monitor, 30° laparoscopic lens, high-definition endoscopic camera system, high-flow pneumoperitoneum, irrigation and suction device, laparoscope, ultrasound equipment, etc. Laparoscopic ultrasonography is very valuable in determining the specific boundaries of the tumor and the detailed anatomy of the blood vessels.
2. Equipment: Choose and use according to the basic conditions of each hospital. Commonly used instruments: ① Electrosurgical instruments, bipolar coagulation, electric hook, argon knife, cutting and closing system, etc.; ② Energy surgical instruments, ultrasonic knife, radio frequency hemostatic knife, microwave knife, etc.; ③ Titanium clip, surgical clip or absorbable Clip (used to clip larger intrahepatic vessels); ④ Endoluminal linear cutting closure device (used for severing hepatic pedicle or hepatic vein, etc.); ⑤ Choledochoscope (used for intraoperative biliary tract exploration); ⑥ Disposable Extraction bag (convenient for the removal of specimens, and for malignant tumors, it can also prevent tumor incision implantation and metastasis).
Laparoscopic liver resection
1. Indications and contraindications for surgery
(1) Indications: Laparoscopic liver resection includes various types of benign and malignant liver lesions suitable for laparoscopic resection.
(2) Contraindications: In addition to the same contraindications as open hepatectomy, it also includes intolerance to pneumoperitoneum.
2. Selection of surgical position, pneumoperitoneum pressure and operating hole
(1)Surgical position: ① Generally, supine position with head high and feet low; ② Whether the patient’s lower extremities are separated can be determined according to the surgeon’s standing position, his own experience and habits; ③ For tumors in the right anterior lower segment or right posterior lower segment of the liver, the patient can use the left side. Lateral position.
(2)Pneumoperitoneum pressure: It is recommended to maintain a carbon dioxide pneumoperitoneum pressure of 12-14mmHg (1 mmHg = 0.133 kPa) to avoid large changes in pneumoperitoneum pressure.
3. Operation hole selection: ① Generally, the 4-hole method or the 5-hole method is used for operation. ② The observation holes are usually located below the umbilicus or around the umbilicus. ③ After pneumoperitoneum is established, the position of the operating hole is determined according to the position of the lesion to be resected. In general, the isosceles triangle principle should be followed between the lesion and the positions of the left and right operation holes, which is conducive to the surgical operation, and the distance between the mirror hole and the operation hole is more than 8 cm. ④ The main operation hole should be as close as possible to the lesion site, the lesion in the right liver should be taken under the xiphoid process, and the lesion in the left liver should be taken under the costal margin of the left midclavicular line.
Three, common surgery
(1) Laparoscopic partial hepatectomy
1. Exploration and free liver: The round ligament and the falciform ligament of the liver are severed in turn, and then the liver is freed according to the lesion site. If the lesion is located in the second segment of the liver, close to the left deltoid ligament and coronary ligament, the above ligaments should be cut off; if the lesion is located in the right posterior lobe, the hepatorenal ligament, right deltoid ligament and part of the right coronary ligament should be cut off to fully expose the lesion.
2. Intraoperative Ultrasound: During partial liver resection, intraoperative ultrasound is necessary. With the help of intraoperative ultrasound, the missed lesions before operation can be found; the tumor location, boundary, presence or absence of sub-focal lesions can be further identified, the relationship between the tumor and the surrounding ducts and the blood vessels on the tangent line can be understood; it is helpful to identify and mark the pre-tangent line.
3. Dissection of liver parenchyma: If the tumor is located on the surface, mark a pre-cut line 1-2 cm from the edge of the tumor; if the tumor is located in the deep part, it is difficult to cut vertically from the liver surface. There is sufficient incision at the base. The liver parenchyma is severed with an ultrasonic scalpel and other liver cutting instruments, and the direction of the cut is maintained. If necessary, intraoperative ultrasound guidance is used to ensure the basal incision margin. In case of large duct tissue, absorbable clips or titanium clips can be used before cutting. To reduce hemorrhage from hepatic venous stumps in liver sections, low central venous pressure techniques can be used.
4. Treatment of liver section and placement of abdominal drainage: after complete resection of the lesion, complete hemostasis on the liver section, bipolar electrocoagulation or argon knife can be used to stop bleeding, and 4-0 to 5-0 non-invasive sutures should be used for active bleeding or bile leakage suture. The liver section can be covered with hemostatic material, and an abdominal drainage tube can be placed.
5. Removal of specimens: The specimens are placed in a disposable collection bag. Small specimens can be taken out directly by expanding the puncture incision. Large specimens can be taken out by making another transverse incision in the lower abdomen or making an incision from the line connecting the two puncture holes under the costal margin. .
(2) Laparoscopic left lateral hepatic lobectomy
1. Exploration and liver dissociation: The round ligament, falciform ligament, left deltoid ligament and left coronary ligament were severed in turn. If there are large blood vessels in the left deltoid ligament, it needs to be clipped and then cut off. The assistant lifted the left lateral lobe of the liver, and the ultrasonic scalpel cut off the lesser omentum to the vicinity of the root of the ligamentum venosum (some patients may not handle the lesser omentum). Sufficient dissociation is crucial for subsequent surgical operations. There is no need to deliberately expose the left hepatic vein or inferior vena cava extrahepatically during the operation.
2. Dissection of liver parenchyma: Start along the left edge of the teres ligament and falciform ligament, use an ultrasonic knife to cut off the liver parenchyma, from the foot side to the head side, from superficial to deep, gradually. The upper and lower liver tissue of segment II/III Glisson sheath was dissected to initially reveal the Glisson branch of segment II/III. When the liver parenchyma is severed, if the larger pipeline is encountered, surgical clips, titanium clips or absorbable clips should be clamped and then cut off.
3. Section II/III Glisson's pedicle: Insert a linear cutting closure device through the main operation hole or right auxiliary hole, and close and cut off the II/III section of Glisson's pedicle.
4. Expose and cut off the left hepatic vein: continue to cut off the liver parenchyma towards the root of the left hepatic vein, cut off the liver tissue above and below the left hepatic vein, expose the root of the left hepatic vein, and cut off the left hepatic vein with a linear cutting and closure device. Damage the diaphragm.
5. Treatment of liver section and placement of abdominal drainage: use argon gas knife or bipolar coagulation to stop bleeding on the liver section, and suture the bile leakage. Optional drainage tube can be used, and a drainage tube is placed under the liver section to puncture a hole on the right side and lead out of the body.
6. Removal of specimens: The specimens are placed in a disposable collection bag. Small specimens can be taken out directly by expanding the puncture incision. Large specimens can be taken out by making another transverse incision in the lower abdomen or making an incision from the line connecting the two puncture holes under the costal margin.
(3) Laparoscopic left hepatectomy
1. Exploration and dissociation of the left hemi-liver: The teres ligament, falciform ligament, left coronary ligament, left deltoid ligament and hepatogastric ligament are dissociated in turn with ultrasonic scalpel or electrocoagulation hook, paying attention to the variant left accessory hepatic artery.
2. Dissection and treatment of the first hepatic hilum: Intrathecal dissection method was used to dissect the left hepatic artery at the entrance to the liver, and then cut it off after clipping with an absorbable biological clip. The left branch of the portal vein was dissociated and blocked with 2-0 silk suture. It is not recommended to separate the left hepatic duct extrahepatically, and the left hepatic duct can be treated when the left hepatic pedicle is severed.
3. Dissection and processing of the second porta hepatis: If the left hepatic vein and the middle hepatic vein join outside the liver, the trunk of the left hepatic vein can be dissected outside the liver and ligated with a 7-gauge silk thread. If it is difficult to dissociate the left hepatic vein, it is not necessary to force extrahepatic dissection. When the liver parenchyma is severed to the root of the left hepatic vein, it should be treated in the liver.
4. Liver parenchyma dissection: Pre-cut lines are marked along the ischemic area of the liver surface. The liver parenchyma was severed to the first porta hepatis with ultrasonic scalpel and bipolar coagulation. The isolated section is the plane composed of the ischemic line on the liver surface, the left border of the middle hepatic vein, and the inferior vena cava. When the liver parenchyma is severed, if the larger pipeline is encountered, surgical clips, titanium clips or absorbable clips should be clamped and then cut off.
5. Dissection of the left hepatic pedicle: As the liver parenchyma is severed, the liver tissue around the hepatic hilum is separated, and the left Glisson's sheath including the left hepatic duct is gradually exposed, which is cut off with a linear cutting and closure device. The left hepatic duct, left hepatic artery and left portal vein can also be dissected separately. In the case of bile duct tumor thrombus, the left hepatic duct should be incised to remove the tumor thrombus.
6. Left hepatic vein dissection: When the liver parenchyma is dissected to the second hepatic porta, the confluence of the left hepatic vein and the middle hepatic vein is exposed, and the root of the left hepatic vein is cut off with a vessel cutting and closing device.
7. Treatment of liver section and placement of abdominal drainage: small oozing blood in liver section can be stopped by bipolar electrocoagulation combined with argon spray coagulation, and active bleeding or bile leakage needs to be sutured; a drainage tube can be selectively placed.
8. Specimen removal: The excised specimen is packed in a disposable collection bag, and the specimen is taken out through the extended umbilicus or a small incision on the pubic bone.
(4) Laparoscopic right hepatectomy
1. Exploration and liver dissociation: cut the hepatic round ligament, falciform ligament, right hepatorenal ligament, right deltoid ligament and right coronary ligament in turn to completely dissociate the entire right liver until the inferior vena cava is exposed. If the right liver or tumor is large and it is difficult to dissociate, it is not necessary to completely dissociate the right liver.
2. Dissection and treatment of the first hepatic hilum: selective right hepatic hilar occlusion, mostly using intrathecal dissection. First dissect the gallbladder triangle, clip and cut the cystic artery and cystic duct, and remove the gallbladder or keep it for traction; longitudinally open the right peritoneum of the hepatoduodenal ligament, dissect the right hepatic artery, and cut it off after clipping with an absorbable biological clip ; Dissect the right branch of the portal vein and ligate it with silk thread; if it is difficult to dissect the right hepatic duct outside the liver, there is no need to force it. At this point, the right hemi-hepatic ischemia line is visible. Extrathecal dissection method can also be used to separate and ligate the right hepatic pedicle along the hepatic hilar plate, but it should be noted that the right anterior and right posterior Glisson's pedicle may not form a common trunk but originate from the trunk respectively.
3. Dissection of the retrohepatic inferior vena cava: The electric hook opens the peritoneum anterior to the inferior vena cava, exposes the short hepatic veins, clamps them one by one from the self-sufficient side to the cephalic side, and then cuts them off. The inferior vena cava ligament was cut to expose the right and anterior walls of the retrohepatic inferior vena cava.
4. Dissection and processing of the second porta hepatis: Completely dissociate the right liver to the right wall of the inferior vena cava, separate the retrohepatic inferior vena cava space cephaladly along the anterior wall of the inferior vena cava, and gently dissect the inferior vena cava from the vena cava lacuna downward. Combined, the main trunk of the right hepatic vein can be separated, and the traction band can be used for backup or cut off with a linear cutting occluder. The dissociation and treatment of the right hepatic vein can also be performed after liver parenchyma with relative safety.
5. Liver parenchyma dissection: The method of liver parenchyma dissection is the same as laparoscopic left hepatectomy. The cut section is the plane of the ischemic line of the liver surface, the right border of the middle hepatic vein, and the midline of the inferior vena cava. Intraoperative ultrasound can be used to determine the course of the middle hepatic vein to help adjust the cut plane. In case of thicker pipes, titanium clips or absorbable clips can be used to clamp them and then cut them off.
6. Dissection of the right hepatic pedicle: As the liver parenchyma is severed, the right hepatic pedicle is gradually exposed, and the right hepatic pedicle is cut off with a linear cutting and closure device. The right hepatic artery, right portal vein branch, and right hepatic duct can also be dissected separately. In the case of intrahepatic bile duct stones or bile duct tumor thrombi, the right hepatic duct should be incised to remove the stones or tumor thrombi.
7. Right hepatic vein exposure and disconnection: When the liver parenchyma is severed to the second porta hepatica, the root of the right hepatic vein is exposed, and the right hepatic vein is closed and cut off with a vascular cutting device.
8. Specimen removal: Put the specimen into a disposable collection bag, and make another transverse incision in the lower abdomen to take it out, or it can also be taken out from the line connecting the two puncture holes under the costal margin. The lower abdominal transverse incision has the advantages of less pain, hidden incision and good cosmetic effect.
9. Liver section processing and placement of peritoneal drainage: close the incision for specimen collection and re-establish pneumoperitoneum. Small oozing blood in the liver section can be stopped by bipolar coagulation combined with argon spray coagulation, and active bleeding and bile leakage need to be sutured. Finally, the falciform and teres ligaments can be sutured to prevent excessive rotation of the left liver to the right. An abdominal drainage tube was placed under the right diaphragm.
Statement: The pictures and texts are from the Chinese Journal of Laparoscopic Surgery. The focus is on the popularization of medical knowledge, and no economic benefits are sought. If there is any infringement, please contact us in time.
Previous
【ENT】Polyps
- Recommended news
- 【General Surgery Laparoscopy】Cholecystectomy
- Surgery Steps of Hysteroscopy for Intrauterine Adhesion
- [General Surgery Laparoscopy] 4K ultra-high definition laparoscopic hiatal hernia repair
- [General Surgery Laparoscopy] 4K Ultra HD Laparoscopic Surgery for Acute Cholecystitis
- [General Surgery Laparoscopy] 4K ultra-high definition laparoscopic deroofing and decompression of renal cysts