【General Surgery Laparoscopy】Basic Techniques of Laparoscopic Surgery
Release time: 18 Jan 2022 Author:Shrek
Patient's position
The operative field of laparoscopic surgery is mainly exposed by the patient's position and pneumoperitoneum. The general principle is to change the patient's position to elevate the target organ, so that the surrounding organs are kept away by gravity, thereby exposing the operative field. For patients undergoing upper abdominal surgery, the head is high and the feet are low, with an inclination of 10°~20°. Under the action of gravity, the bowel is moved to the lower abdomen and pelvis, which is conducive to the exposure and operation of the surgical field, such as laparoscopic cholecystectomy, common bile duct incision, and gastrectomy. , splenectomy, partial liver resection, etc., according to the needs of the operation, the right side is slightly raised or the left side is slightly raised. Lower abdominal surgery patients generally need to use the head down and feet high, and the operating table is inclined 10°~30° to the head side, which is conducive to the transfer of abdominal internal organs to the upper abdomen, and the pelvic cavity is empty, which is conducive to the exposure and operation of the surgical field. It is usually suitable for hernia repair, appendix Resection, rectal resection, etc. According to the needs of the operation, the right side is slightly raised or the left side is slightly raised. Sometimes the patient can also take the Lyold-Davis position, the lower limbs are separated, the knees are slightly flexed, and the legs are placed on the stent, which is suitable for laparoscopic anterior resection of rectal cancer. This position is also suitable for laparoscopic surgery on the upper abdomen and thyroid gland. The operator is more comfortable to stand between the patient's legs than to one side, and the assistant stands on both sides to facilitate the operation.
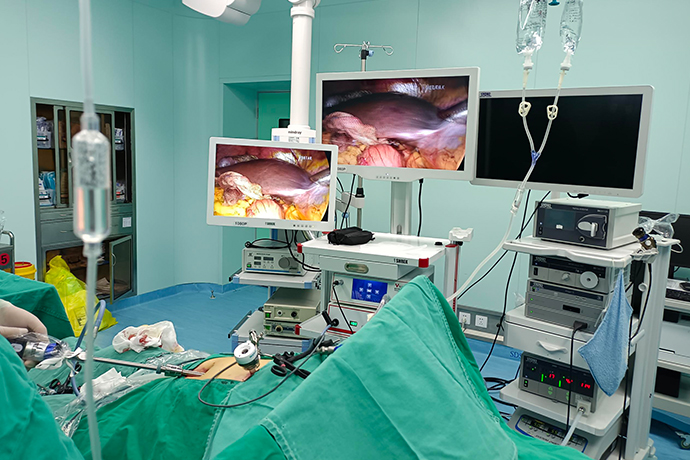
Establishment of pneumoperitoneum machine
There are two methods of intra-abdominal inflation: closed inflation and open inflation.
(1) Closed inflation method
In the closed inflation method, the pneumoperitoneum needle inflation method is the most commonly used method. The principle of puncture point selection requires that after the laparoscope is inserted, it is convenient to observe the surgical site in the abdominal cavity and explore other parts of the abdomen; the puncture point has few blood vessels; the puncture point has no intestinal tube adhered to the abdominal wall. Generally, the upper or lower edge of the umbilicus is taken as the piercing point. During the puncture, the patient is lying supine, and two towel forceps are used to clamp the fascia and the skin on both sides of the puncture point, and the abdominal wall is fully lifted so that there is enough space between the abdominal wall and the organs. Line) or arc (upper umbilicus or lower umbilical edge) 1cm small incision, gently pinch the pneumoperitoneum needle with the right thumb and index finger, twist the wrist forcefully when the needle is inserted, and there is a feeling of loss after piercing the peritoneum. Do not use too much force during needle insertion to prevent the needle from protruding too deep into the abdominal cavity and damaging the bowel. To confirm whether the pneumoperitoneum needle has penetrated into the abdominal cavity, one is to use a syringe to suck a small amount of water, connect the pneumoperitoneum needle, and the water is sucked, indicating that the abdominal cavity has been penetrated; Low-flow inflation, if the intra-abdominal pressure is about 3mmHg, it also means that the abdominal cavity has been penetrated; third, when inflating, pay attention to whether the abdomen is evenly and symmetrically expanded.
(2) Open inflatable method
The open inflation method is to make a small incision of about 2cm at the puncture point, and cut it layer by layer until the peritoneum is cut through, and then use two towel forceps to lift the abdominal wall on both sides of the incision, and gently insert the abdominal cavity with a 10mm blunt cannula. The sutures on both sides are knotted to fix the cannula and the abdominal wall, and at the same time prevent gas from leaking out, and an air inlet switch is also arranged on the blunt cannula. The use of blunt cannula inflation method can avoid accidental peritoneal intestinal injury. The blunt cannula is also called Hasson cannula. This method is safer because the tube is placed under direct vision. Therefore, as long as the method is correct, there is almost no intestinal injury. Danger. Generally used for patients with intra-abdominal adhesions.
Cannulation technology and positioning of the legendary cannula
Laparoscopic surgery must establish a human abdominal channel, including observation mirror channel, surgical channel and exposure channel. The observation mirror channel is the channel for inserting the laparoscope. The surgical channel is used to insert coagulation hooks, dissecting scissors, ultrasonic knives, and cutters. It is the main channel for operation, also known as the "main operation hole". The exposure channel is used for inserting non-invasive grasping forceps and retractors to pull and expose the operation object, also known as "auxiliary operation hole". To establish a human abdominal channel, the insertion of the puncture cannula must be performed first. Insertion of puncture cannula: There are three basic types of puncture cannulae commonly used, reusable pointed puncture cannula, disposable puncture cannula with safety sheath, and blunt puncture cannula. The reusable pointed puncture cannula does not have a safety sheath, and its pointed end is always exposed during the entire puncture process. Using this puncture cannula for the first transumbilical puncture has the risk of damaging abdominal organs or large retroperitoneal vessels.The disposable puncture cannula is attached with a safety sheath to reduce the probability of abdominal organ damage. The first cannula is mostly used to insert the laparoscope, usually around the umbilicus, and the closed intubation method is often used. When the cannula is inserted, the skin and subcutaneous tissue on both sides of the incision are clamped with two cloth forceps, and the two sides of the abdomen are flattened. Pull to fix the abdominal wall, the operator presses the volar enlargement of the trocar cone with the right palm, so that the tip of the needle cone protrudes from the front end of the cannula for puncture, the right index finger is straight and placed on the side of the cannula to prevent the cannula. When a person's abdomen is too deep and the internal organs are damaged, the remaining four fingers hold the cannula respectively, and use the wrist force to turn and press the cannula down. Cone, if gas escapes, it proves that the cannula has entered the abdominal cavity. It is estimated that there is adhesion between the abdominal organs and the abdominal wall, and the open abdominal approach can be used. The second, third, and fourth puncture process, because the surgeon operates under the laparoscopic direct vision, as long as the operation is done properly, there is generally no danger. The positioning of the puncture cannula: The positioning of the puncture cannula has a great relationship with the success of laparoscopic surgery. The positioning of the puncture cannula is not only conducive to the operation, but also has the concealment and cosmetic effect. Care should be taken to avoid organs such as larger nerves, blood vessels, and bladder in the abdominal wall.The puncture port should be made as much as possible to make a transverse skin incision, consistent with the direction of the dermatoglyphics. The first puncture cannula is usually used for the entry and exit of the sight glass, and its location is mostly selected at the umbilicus. For the laparoscope placed in the abdominal cavity through the first cannula, a visual inspection of the abdominal cavity is performed first, and then the positioning of other puncture cannulas is determined according to the results of the inspection, which should be determined according to the operation. In general, for most laparoscopic surgeries, it is ideal to choose the position of the viewing scope out of the human cannula at the umbilicus. If you want to observe the hand side from different perspectives, according to the principle of bisecting triangle, the angle between the two manipulating arms is ideal, and the angle between the two manipulating arms should be equally divided by the axis of the observation mirror, which is helpful for the operator to grasp the two-dimensional image. direction, the operation is more convenient.
Laparoscopic support
The observation mirror should not enter the abdominal cavity too quickly, but should be entered carefully and slowly. The positioning should be selected in a place with less interference from unrelated organs and instruments. The abdominal organs that affect the visual field should be removed by appropriate patient positions or retraction instruments. Avoid interfering with the surgical field. There is a fine focus adjustment knob on the camera, which can be adjusted manually. The scope arrives at the surgical site for a close-up image, and zooms out for a wide-angle or "panoramic" image. The scope should be moved slowly and carefully in the abdominal cavity. Moving too fast will cause the image to be dislocated and shaken, and it will also make the surgical team feel "seasick". The hand holding the mirror should be steady, otherwise the image will shake up and down, and it will also make people dizzy. Observation of mirror fogging is a common problem encountered during surgery. The reason is that the temperature of the abdominal cavity and the mirror surface is different, which causes water vapor to condense on the mirror surface. The mist liquid is applied to the mirror surface to avoid fogging of the mirror surface. Although the "cold light source" is used, the light passing through the light guide channel of the sight glass will still make the lens hot. If the laparoscopic lens is directly aimed at the target, the high temperature of the lens can sometimes cause the surgical towel to burn, so the lens holder should always Know the position of the lens to prevent the lens from being too close to the bowel and causing burns to the bowel wall.
Separation technology
Like conventional open surgery, the dissection technique in laparoscopic surgery is one of the most basic operations in surgery, which separates the diseased tissue to be resected from the surrounding normal tissue by dissection. There are blunt separation, sharp separation, electric knife separation, ultrasonic knife separation and laser separation, high pressure water separation.
(1)Blunt dissection Blunt dissection is to separate the tissue to be separated with separation forceps, and separation rods or even irrigation tubes can also be used for separation. When separating, try to start from the visible tissue gap or loose tissue, and insert the separation forceps into the gap for expansion. When expanding, the force should be moderate and gradually enter to avoid tearing the adjacent blood vessels and organs. (2) Sharp separation Sharp separation of laparoscopic surgery is usually performed with long curved scissors. Tissues with no or few blood vessels can be separated and cut open with scissors. Tissues with small blood vessels can be clamped with scissors first, and then cut after coagulation and coagulation. Sharp separation is more delicate than blunt separation, and the operation should be precise and performed under the premise of a clear field of view, avoiding blood vessels to avoid heavy bleeding. (3) Electro-knife separation Electro-knife separation is the most common separation method in laparoscopic surgery. It can coagulate blood vessels and cut off tissues. In most cases, electric hooks are used for separation. When separating, first thinly hook the tissue to be separated, confirm that there is no important tissue structure, and then perform the electric cut. Do not use electrocautery to separate large pieces of tissue and continuously electrify the separation or coagulation to avoid thermal burns to the surrounding important tissues. If bleeding occurs in the separation of the gallbladder triangle, do not use continuous or blind coagulation, but absorb the oozing blood. After the surgical field is clear and important structures such as the common bile duct are identified, intermittent coagulation or separation should be used.(4) Separation of ultrasonic knife The ultrasonic knife can significantly reduce the amount of blood loss and operation time in operations with more complex operations such as laparoscopic gastrointestinal tract, and reduce the difficulty of operation, making it possible to popularize it. In the current endoscopic thyroid surgery, ultrasonic scalpel shows its incomparable superiority. For small blood vessels under 2mm, there is no need to separate the blood vessels first. You can choose a blunt cutter head and a medium-speed gear, and use a scissors-shaped cutter head to cut at one time; for larger arterial and venous blood vessels of 2~3mm, you can use The breakwater technique is to use a scissors-shaped cutter head to coagulate the near side of the blood vessel where it is to be cut without cutting it. Repeat several times until the tissue turns white to confirm that the blood vessel has been coagulated. Length, thicker blood vessels coagulate longer, generally up to 5 ~ 10mm, and then coagulate and cut the blood vessels at the place to be cut. When separating close to important structures (such as blood vessels, nerves, etc.), the functional cutter head surface of the ultrasonic scalpel should pay attention to avoid these structures and use a fast speed to cut and separate.
Ligation technique
Laparoscopic surgery, like conventional open surgery, requires ligation of tubular structures such as large blood vessels and cystic duct. The methods of ligation include clipping method and wire tying method. (1) Clipping method The easiest ligation method in laparoscopic surgery is the clipping method, which is generally only used for the ligation of small blood vessels and thinner cystic ducts. There are metal clips and bioabsorbable clips, the latter being more expensive. Metal clips sometimes slip off, so it is more secure to use double clips. The front end of the bioabsorbable clip has a barb, which is not easy to fall off after clamping, so one clip is enough. No matter which kind of clip is used, when applying the clip, it must be judged that the structure to be clamped can be completely clamped, and the clip should be perpendicular to the structure to be clamped, not at an oblique angle. Before clipping, the operator must see the end of the clip clearly to prevent other tissue deep into the structure to be clipped by mistake. The clip appliers can be reusable and need to be reloaded after each clip application; they can also be disposable, with a "magazine" for clipping, which can be applied continuously, but the price is slightly more expensive. The clip applier can apply the clip from the end or from the side.
The suture theorem under laparoscopy mainly has the following four points:
1. Suture is the operation of pulling the thread from the tip of the needle through a certain tissue, which can be formed by single (intermittent) or multiple (continuous), etc. or a combination of many.
2. The curved needle with a certain arc is designed according to the rotation of the wrist, which is easy to operate finely and smoothly.
3. Under the lens screen, the curvature of the looper forms a surface, which needs to be perpendicular to the mouth of the needle holder (clamped and fixed), and also needs to intersect with the vertical plane of the long axis of the needle holder. The angle is between 90-128 degrees to be sutured.
If the curved surface of the looper and the B surface are not within this angle range, the stitching operation will be very difficult, and even the stitching operation will not be completed.
4. Under the camera screen, if you use a straight needle to sew, the space dimension of one face is reduced compared with a curved needle.
The suturing action can be done by adjusting the angle between the straight needle and the needle holder between 90-128 degrees.
Therefore, for laparoscopic operators, suture with straight needles can visually reduce the dimension and reduce the difficulty. This makes some sense.
Knotting Tips
Once the knot is not tied tightly, all previous efforts will be lost, so surgical knots should be tied under the microscope
"The first knot is strictly forbidden to cross"
Be familiar with the direction of the pull wire to prevent the first knot from crossing
Go with the flow - follow the "temperament" of the line
Both hands must be able to tie knots
The difficult part of knotting under the mirror lies in the "clamping tail"
stitch + knot
Forehand stitching, right hand knotting (1): The right needle is held on the thread and looped, so the right needle is held down when the hands are crossed.
Forehand stitching, right hand knotting (2): The right needle is held under the line and looped, so when the hands are crossed, the right needle is held on top.
Forehand stitching, left hand knotting (recommended): No need to cross your hands when tying the knot, saving space and being calm and natural.
Backhand stitching, right hand knotting: The hands do not need to be crossed when pulling the knot, the same effect as before.
Knotting when "barbed seam": "barbed seam" is equivalent to backhand stitching, so there is no need to cross the knot with the right hand.
- Recommended news
- 【General Surgery Laparoscopy】Cholecystectomy
- Surgery Steps of Hysteroscopy for Intrauterine Adhesion
- [General Surgery Laparoscopy] 4K ultra-high definition laparoscopic hiatal hernia repair
- [General Surgery Laparoscopy] 4K Ultra HD Laparoscopic Surgery for Acute Cholecystitis
- [General Surgery Laparoscopy] 4K ultra-high definition laparoscopic deroofing and decompression of renal cysts