【General Surgery Laparoscopy】Exploration Through the Bile Duct
Release time: 12 Jan 2022 Author:Shrek
Improvement and popularization of biliary surgery
In the past two decades, the development of biliary surgery has made extraordinary achievements. However, compared with the liver surgery and pancreatic surgery in the same period, it is still inferior. Biliary tract surgery, in which cholangiolithiasis is the disease with the highest incidence, with a large number of patients, the main treatment method is still cholecystectomy, and the introduction of laparoscopic technique is only to add a new surgical technique, its treatment Exactly the same as the treatment of gallstones more than 100 years ago. Research on stone prevention is still lingering. Recent studies on the susceptibility genes of cholelithiasis families and patients with cholesterol stones have not revealed the whole picture of the mechanism of cholelithiasis, which is a subject to be focused on.
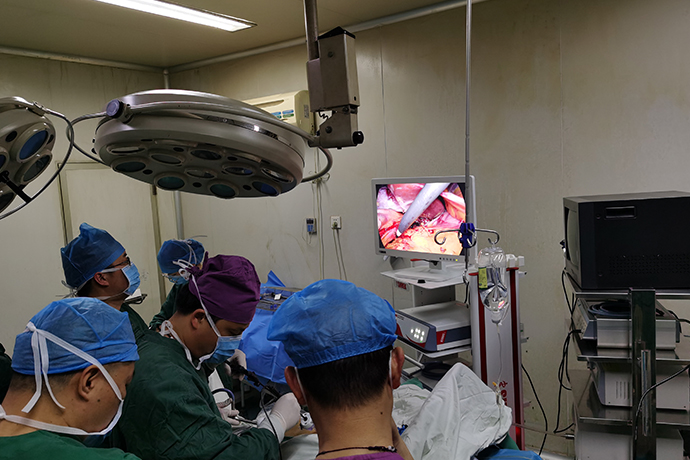
Biliary tract surgery is a must-have operation, but unplanned reoperations also greatly trouble the surgeon. Due to the lack of understanding of the principles of surgery, unclear goals, and insufficient estimation of difficulties, resulting in residual stones, biliary tract injury, unreasonable surgical methods, and wrong surgical methods for biliary tract reoperation, it is necessary to strengthen the theoretical knowledge of biliary tract surgery and the study of surgical experience.
The history of biliary surgery
In the past decade, the treatment of biliary tract surgical diseases has made great progress. Especially with the development of laparoscopic surgery, combined with other minimally invasive techniques, new breakthroughs have been made in the treatment of biliary tract surgery.
Laparoscopic transcholedochal exploration (LTCD) represents the most versatile surgical approach for the treatment of choledocholithiasis. Originally based on the gold standard technique for open common bile duct exploration, the transbiliary approach has gradually developed into an effective and safe option for the treatment of patients with choledocholithiasis in the laparoscopic era. Compared to transgallbladder access, LTCD provides potential access to the entire proximal and distal biliary system, eliminates the need for cannulation and devices necessary to dilate the cystic duct, and can be used to remove stones of any size or occasional Devices trapped in previously failed devices Endoscopic or percutaneous procedures. However, LTCD is more technically challenging than transcystic exploration and has a higher risk profile, so proper patient selection and attention to technical details are important to ensure optimal outcomes.
The indications for LTCD are similar to those for transcystic exploration, including patients with preoperative or intraoperative confirmed choledocholithiasis. LTCD can be used as a primary strategy in patients in whom laparoscopic general duct debridement or transgallbladder approach has failed or is not feasible. LTCD is well suited for patients who have concurrent cholecystectomy, but in some cases surgery can even be performed after prior cholecystectomy (unlike transcholecystectomy). When endoscopic retrograde cholangiopancreatography (ERCP) is not possible or most commonly in patients with difficult or failed ERCP (eg, previous gastric bypass with Billroth II or Roux-en-Y). The surgeon performing LTCD should have a high degree of confidence in the diagnosis of choledocholithiasis compared to performing transcapsular exploration, however, because LTCD represents a technically more challenging procedure, requires laparoscopic suturing skills and has high risk characteristics.
To avoid the development of biliary strictures, it is recommended to avoid choledochotomy in patients with small diameter bile ducts (<7 mm) even when T-tubes are used. If the bile duct is larger than 3 mm, or if endoscopic stone removal is performed, transcholecystic exploration is preferred for patients with small-diameter bile ducts.
Informed consent prior to any cholecystectomy should include the possibility to request laparoscopic common bile duct exploration. If transbiliary exploration is possible, the risk of bile leakage, bile duct injury, and bile duct stricture should be discussed, as well as the possibility that the patient may require internal (biliary stent) or external drainage (T-tube or closed drain) or a second Surgery (eg, ERCP or subsequent esophagogastroduodenoscopy (EGD)) (removal of biliary stents if used).
Cholangiography
In most cases, routine intraoperative cholangiography through the cystic duct is strongly recommended, as this will delineate the anatomy of the bile duct and the location of the stone and provide a roadmap for exploration.
bile duct incision
Once the decision is made to proceed with transbiliary exploration, the surgeon may stay on the patient's left side or move to the patient's right side and place an additional trocar in the lower right quadrant between the outermost trocar and the surgical needle . The camera facilitates dissection. Operation from the right side provides a comfortable angle for tracheotomy and suturing. When the surgeon is on the right side, the surgeon uses the outermost trocar plus the trocar in the lower right quadrant, while the assistant moves to the patient's left side and uses the subxiphoid trocar to retract the head of the gallbladder . The superior duodenal common bile duct can be seen as a blue-green tubular structure on the right anterior side of the hepatic hilum. The peritoneal covering of the hepatoduodenal ligament should be incised anterior to the bile duct, and a flat blunt dissection should be used to expose the bile duct. Dissection along its lateral and medial sides should be avoided, and attempts to circumnavigate the bile duct should not be attempted so as not to injure the "3 o'clock" and "9 o'clock" arteries that supply air and run parallel to the bile duct. Exposure should be sufficient to allow a 1–2 cm longitudinal incision on the catheter. If there is doubt about the location of the bile duct, a fine needle can be used to aspirate the bile to confirm the location of the bile duct. Longitudinal incisions are preferred so as not to interrupt the blood supply to the common bile duct.The incision can be made with a laparoscopic knife or fine scissors. Indwelling sutures are often unnecessary and risk being pulled, tearing the catheter. Due to the ability of the CBD to expand and stretch, the incision length should generally be kept less than 1.5 cm. Remember not to make the incision on the right side of the midplane of the duct to avoid the incision into the cystic duct - a common ductal septum that occurs in about 20% of patients when the cystic duct runs parallel to the normal duct.
Stone extraction
Extracting stones through a choledochotomy can be done in a number of ways. In general, it is recommended to start with the simplest operations and progress to more complex operations if necessary:
1. Irrigation: The surgeon places the tip of a suction irrigator into the choledochotomy to irrigate the catheter. Small stones and debris can be easily removed with this simple maneuver, and larger, free-floating stones can be pulled toward the choledochotomy by following the flow of saline. Once seen at the choledochotomy, these larger stones can be grasped and removed. A 14F red rubber catheter can also be inserted into a 5 mm trocar and threaded distally or proximally and flushed vigorously as it is withdrawn to clear more distant stones.
2. Balloon Removal: The Fogarty Balloon Catheter or ERCP Stone Removal Balloon, which is passed through the wire (located on the nipple), is passed through the choledochotomy and guided distally. The balloon is guided over resistance and then slowly withdrawn and inflated, then gradually withdrawn through a choledochotomy to remove debris. This technique may require multiple passes through the balloon to remove all debris.
Closure
In simple cases, only one primary closure is sufficient, in which there is little to no manipulation of the nipple, no purulence in the bile duct, and little concern in calculi and relatively healthy patients. The catheter can be closed intermittently or continuously using fine absorbable 4-0 sutures such as Vicryl (polylactic acid 910) or PDS (polydioxane). Compared to interruption techniques, running techniques offer greater convenience. Suture bites should be full thickness, approximately 1-2 mm from the incisal edge of the catheter, and spaced every 2 mm. Sutures should be tested by flushing saline through the cystic duct using a cholangiography catheter while observing saline leakage. Place additional interrupted sutures where the leak occurred and recheck closure. Closed cholangiography should also be performed to check for extravasation of contrast media and to confirm duct patency and filling defects. The main advantage of primary closure is that the patient does not require prolonged T-tube drainage and avoids the potential discomfort and potential complications associated with T-tubes. However, one of the downsides of primary closure is that the risk of bile leakage may be greater if bile duct compression is performed postoperatively, as in extensive nipple manipulation or when the risk of retaining stones is high. Bile drainage may also be impaired in cases of ampullary edema or cholangitis. However, in carefully selected patients, there is evidence that the technique reduces operative time, shortens hospital stays, and may actually have lower complication rates than T-tube closure.
T-Tube Closed
U-tubes are a traditional adjunct to choledochotomy and are commonly used by some surgeons, including the senior author. Conventional users believe that common bile duct instruments and procedures for stone removal may cause papilledema and increased pressure within the biliary tree, creating an environment that puts the seal at risk of bile leakage. The placement of the T-tube resolves edema and spasm while preventing cholestasis. In patients with cholangitis, ensuring continuous drainage of bile is especially important to prevent recurrent cholangitis and ensure resolution of sepsis. The T-tube also provides continuous access to the biliary system for interval cholangiography, removal of any remaining stones, or to facilitate subsequent ERCP sampling. The advantage of the T-tube technique over the use of an internal biliary stent is that the biliary prosthesis can be removed by simply pulling the T-tube at the bedside without the need for additional endoscopy as with biliary stents. Although gallbladder drainage (as an alternative to a T-tube) can also be performed in some patients, placement of a T-tube into the common bile duct is more extensive and will be the only technique described. The sizes of T-tubes used by surgeons vary, with some surgeons advocating the use of 14F T-tubes to make percutaneous intervention easier if needed. The senior author prefers the 8F tube because it reduces patient discomfort and requires a smaller bile duct opening. A T-tube is made by trimming the crossbar of the T to approximately twice the size of the choledochotomy of a long and short limb. The crossbar segment is then cut longitudinally to open the posterior wall, and a long tube is then inserted into the catheter in the distal catheter. The choledochotomy was closed in a continuous fashion using a 4-0 Vicryl continuous suture. The first bite is the most important, be careful not to stick to the test tube so as not to combine with the test tube. The first bite should keep the tube snug against the pipe, which is critical for anchoring the tube and preventing migration or leakage. Subsequent bites move in a caudal direction until the catheter is fully closed. The T-tube was then externalized through one of the 5 mm trocar sites in the upper right quadrant at the end of the surgical procedure. It is important to allow a small amount of slack in the tube so that postoperative bloating does not create tension on the tube and cause it to dislodge. Even if a T-tube is placed, it is recommended to place a closed suction port near the T-tube to help detect and control possible postoperative bile leakage. Although post-operative T-tube management varies widely among surgeons, most surgeons leave the tube in place for at least 2 to 6 weeks.
The senior author's technique using the 8F T-tube will be described. After surgery, the surgeon places the drainage bag on the floor for about 12 hours while examining the closed suction port for signs of bile leakage. If drainage is poor, reposition the T-tube in a horizontal position on the bed for another 12 hours. After this time, place the bag at the head of the bed. If no bile is visible in the closed suction port, clamp the T-tube. It is believed that this method, with its various positional variations, may allow testing of the integrity of the repaired choledochotomy by sequentially changing the intraductal pressure. The closed drain was then removed before discharge, and the patient was scheduled for cholangiography 10-15 days postoperatively. If there are no residual stones or bile leakage, remove the T-tube. If retained stones are present, they are removed endoscopically.
primary biliary closure
Primary closure with a biliary stent is a relatively new technique that combines the simplicity of primary closure with the internal drainage provided by a transampulla stent. The surgeon inserts a biliary stent through the choledochotomy before the choledochotomy is closed. A laparoscopic 7F biliary stent (Fanelli stent, Cook Medical) can be used, or an 8.5F biliary stent designed for ERCP deployment can be used. If an ERCP-type stent is used, it is recommended to secure its pre-fixed 5–7 cm stent to the delivery catheter with sutures and to be able to be repositioned by withdrawing the catheter. The surgeon obtains wire access through the nipple and then loads the stent delivery system back onto the wire. Stent delivery systems typically have fluoroscopic markers positioned across the nipple, and once in place, the stent is deployed. Choledochoscopy can be used to confirm the position of the stent across the nipple from the side of the common bile duct. The stent does not need to straddle the choledochotomy closure site, but serves to ensure continued internal drainage after the choledochotomy is closed to prevent compression of the bile duct and the potential for bile leakage as a result. Once the stent was in place and the choledochotomy was closed, the surgeon performed a cholangiography to confirm the watertight closure of the choledochotomy and the absence of a filling defect. A closed drain is placed near the closure of the choledochotomy to monitor postoperative bile leakage. The drain is usually removed before the patient is discharged from the hospital. The EGD was planned to be removed from the biliary stent after 2 to 4 weeks in the outpatient clinic. Using a foreign body forceps or snare, the stent is removed using a standard gastroscope. A clear cover can be fitted to the end of the gastroscope to facilitate visualization of the nipple and to grasp the holder if necessary.
Precautions
1. Bleeding is mainly caused by inadvertent damage to the variant cystic artery, right hepatic artery, and hepatic artery and vein. Occasionally, the portal vein runs before the common bile duct. If the common bile duct is not carefully dissected along the cystic duct, and the possibility of the portal vein is not ruled out by puncturing first, once it is mistakenly identified as the "common bile duct" of the portal vein, it will lead to massive hemorrhage and endanger the patient's life. In addition, puncturing the common bile duct with a sharp knife is easy to penetrate the anterior and posterior walls of the common bile duct, and even injure the portal vein behind the common bile duct. Improper use of electric hooks and scissors around the dissection of the bile duct can also damage the surrounding important blood vessels, resulting in bleeding. 2. The main reasons for bile leakage include loose suture around the T-tube, undiscovered treatment of the variant accessory bile duct or vagal bile duct injury, residual stones or strictures at the lower end of the bile duct. 3. The incidence of residual bile duct stones is higher in emergency surgery and when there are many bile duct stones. After 6 to 8 weeks after the T-tube sinus is completely formed, choledochoscopy can be used for lithotripsy. 4. Residual calculi in the abdominal cavity are mostly caused by multiple and fragile calculi, not placing gauze in the Wen's hole, and failing to put the removed calculi into the specimen bag in time. Stones remaining in the abdominal cavity can become the main cause of abdominal infection and intestinal adhesions. 5. Peripheral organs that are easily damaged by visceral injury include duodenum, transverse colon, stomach, liver, and diaphragm. The main reasons are improper use of electrosurgery, insufficient bowel preparation, and rough and irregular technical operations.
- Recommended news
- 【General Surgery Laparoscopy】Cholecystectomy
- Surgery Steps of Hysteroscopy for Intrauterine Adhesion
- [Thoracoscopic Surgery] Thoracoscopic Radical Resection of Lung Cancer
- [General Surgery Laparoscopy] 4K ultra-high definition laparoscopic hiatal hernia repair
- [General Surgery Laparoscopy] 4K Ultra HD Laparoscopic Surgery for Acute Cholecystitis