【General Surgery Laparoscopy】Right Hepatectomy
Release time: 30 Nov 2021 Author:Shrek
Laparoscopic right hemihepatectomy is a highly technically difficult surgical operation. The main reason is that the procedure is complicated, there are many liver anatomical variations, intraoperative bleeding is common, and bleeding that is difficult to control is prone to occur, and the incidence of intraoperative and postoperative complications is high.
The world's first laparoscopic hepatectomy successfully implemented by Reich et al. in 1991 opened a precedent for the clinical application of laparoscopic technology in liver surgery. In 1994, Zhou Weiping reported the first laparoscopic liver tumor resection in China. In 1997, Hüscher et al. first reported laparoscopic right hepatectomy in the world.
In 2004, Nibcolas and others of the Royal Hospital of Brisbane, Australia, reported 12 cases of laparoscopic right hepatectomy, 5 of which were successful. This is the first group of multiple cases reported in the world. Cai Xiujun and others first reported the successful completion of a complete laparoscopic right hepatectomy in China in January 2005. After 2005, reports of laparoscopic right hepatectomy continued to increase, the operation time was gradually shortened, and the rate of conversion to laparotomy was also gradually reduced.
Although laparoscopic right hepatectomy is still one of the relatively complicated laparoscopic liver resections, with the advancement of laparoscopic hepatectomy technology, laparoscopic right hepatectomy is also increasingly used The treatment of liver disease has become a routine standard procedure even in many larger liver surgery centers at home and abroad.
In addition, in the area of donor liver harvesting for living donor liver transplantation, in 2006, Koffron et al. first reported the right hemiplegic liver harvesting for living donor liver transplantation assisted by laparoscopic surgery in the world. In 2013, Soubrane et al. and Rotellar et al. respectively reported complete laparoscopic living donor liver transplantation and the right hemiplegic liver resection. At present, a few liver transplant centers in China, such as the General Hospital of the People's Liberation Army and West China Hospital of Sichuan University, have carried out total laparoscopic living donor liver resection. However, the number of patients is small and it is still in its infancy.
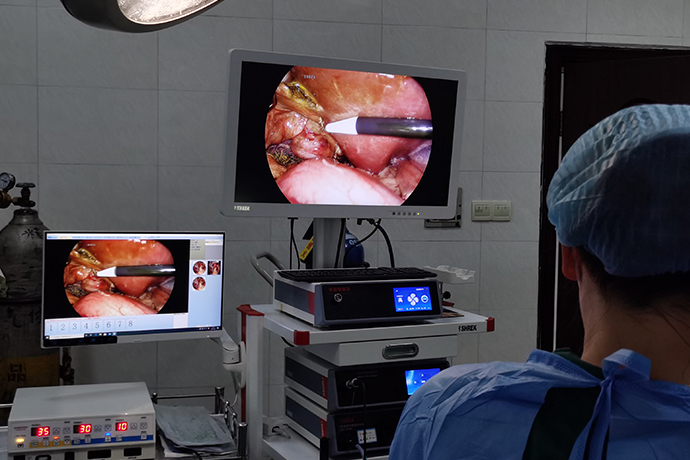
1. Surgical approach
The surgical approach of laparoscopic right hepatectomy is divided into two types: conventional approach and anterior approach. At present, most liver surgery centers in China adopt a conventional approach, that is, fully free the surrounding ligaments of the liver, handle the short hepatic blood vessels and even the right hepatic vein, and dissociate the liver parenchyma under sufficient exposure conditions to prevent the liver parenchyma from being dissected to a deeper position. The bleeding was difficult to fully reveal and control, resulting in forced transition to open abdomen.
The team of Professor Chen Yajin from Sun Yat-sen Memorial Hospital of Sun Yat-sen University routinely cut the liver through an in-situ anterior approach, cut off the liver parenchyma from bottom to top, from shallow to deep, finely dissected the intrahepatic ducts along the "intrahepatic space", ligated one by one, and finally processed the perihepatic ligament . They believe that this surgical method is more in line with the principle of tumor-free laparoscopic right hepatectomy for liver cancer. This standardized operation has played an active role in the promotion and application of laparoscopic right hepatectomy.
2. Surgical indications and contraindications
In terms of disease spectrum, the indications of laparoscopic right hepatectomy are basically the same as open surgery, including benign and malignant tumors involving the right hepatic liver, inflammatory lesions, right intrahepatic bile duct stones, and cystic bile duct confined to the right liver Expansion, etc., and even the right half of the donor liver for living donor liver transplantation. However, the current laparoscopic surgery method cannot completely replace the open surgery method.
In 2013, the "Expert Consensus on Laparoscopic Hepatectomy" formulated by the Liver Surgery Group of the Chinese Medical Association Surgery Branch proposed that the indications for laparoscopic liver resection: benign diseases include symptomatic or spongy with a maximum diameter of more than 10 cm Hemangioma; symptomatic focal nodular hyperplasia or adenoma; symptomatic or hepatic cyst with a maximum diameter of more than 10 cm, intrahepatic bile duct stones, etc.
Liver malignancies include primary liver cancer, secondary liver cancer and other rare liver malignancies. Contraindications include in addition to contraindications for open right hepatectomy, but also those who cannot tolerate pneumoperitoneum; those with intra-abdominal adhesions that are difficult to separate and expose the lesion; those whose lesions are close to or directly invade large blood vessels; The second or third hepatic hilum affects those exposed and separated; the hilar is invaded or the lesion itself requires extensive hilar lymph node dissection.
In view of the high risk of laparoscopic right hepatectomy, the indications should be selected to facilitate the anatomy of the first hepatic portal and the treatment of the second and third hepatic portals. Therefore, the indications for laparoscopic right hepatectomy should be open On the basis of right hepatectomy, the following conditions are excluded:
⑴ The lesions near the hepatic hilum;
⑵ Liver cirrhosis is obvious, liver cancer with abundant collateral circulation at the hilar;
⑶ Repeated episodes of cholangitis, leading to obvious fibrosis of the right intrahepatic bile duct stone disease in the hilar area. In recent years, with the continuous advancement of laparoscopic liver resection technology, the indications of laparoscopic liver resection have been continuously expanded, and some of the contraindications considered in the past have become relatively contraindications or even non-contraindications.
The author believes that, theoretically, the indications of laparoscopic right hepatectomy have been highly close to open surgery, but we should realize that the development of laparoscopic hepatectomy is unbalanced. Due to the uneven surgical techniques of surgeons, indications and contraindications are not applicable to every surgeon in liver surgery. Individuals should choose the surgeon's personal surgical indications under the premise of fully ensuring the safety of the patient.
3. Surgical methods and steps
(1) Patient position and card layout: The patient is in a supine position, the right posterior hepatic area is raised 30°, the right arm is suspended, general anesthesia, and the five-hole method is used. An incision was made 2 cm to the right of the umbilicus to establish a pneumoperitoneum, a 10 mm punch card was inserted, and a 30° laparoscope was inserted, 2 cm below the xiphoid process, 5 cm above the umbilicus at the midline of the abdomen, and 6 cm below the costal margin of the right midclavicular line, respectively A 12 mm disposable poke was inserted into the incision, and a 5 mm disposable poke was inserted into the 2 cm incision below the costal margin of the right anterior axillary line.
Using the dual main knife operation mode, the surgeon on the right side of the patient holds the separating forceps or Beike forceps in the left hand to hold the separated liver to help expose, and the right hand holds the ultrasonic knife or CUSA to cut the liver parenchyma. The surgeon on the left side of the patient holds an ultrasonic knife, bipolar electrocoagulation, or aspirator to operate.
(2) Disconnected ligament: After laparoscopic exploration judges that there is no distant metastasis feasible for surgical treatment, the perihepatic ligament is disconnected. The order is generally hepatic round ligament, falciform ligament, right triangular ligament, right coronary ligament, liver and kidney ligament .
(3) Routine resection of the gallbladder and anatomy of the first hepatic hilum: The author advocates intrathecal anatomy. Dissect the Glisson sheath of the hepatoduodenal ligament from the right side of the common bile duct, gradually open the peritoneum, and identify the portal vein along the posterior space of the common bile duct.
There is a loose gap between the two. Separate this gap from the side, remove or separate the lymph nodes on the right side of the portal vein, and look for the main stem of the right branch of the portal vein to the head. The separation of the portal vein should expose a part of the main trunk and suspend it, which is helpful for the judgment of the left and right branches of the portal vein and the continuous blockage of the portal vein trunk during the subsequent process of separating the liver parenchyma.
Note that after opening the gap between the portal vein and the bile duct, close the separation of the portal vein. The anatomy of the right branch of the portal vein is generally by the left main knife and the right hand holding a large right-angled forceps to poke the card hole under the xiphoid process, enter through the front side of the left and right branches of the portal vein, take out from the dorsal side of the right branch of the portal vein, and then hang it with silk thread , The proximal upper vascular clip is clamped, and the distal end is not cut temporarily.
During the separation process, after opening the lateral and dorsal serous membranes of the portal vein, be aware that there may be branches leading to the caudate and square lobes, and be careful to avoid tearing and bleeding during the separation process. After fully exposing these branches, the branch from the right portal vein to the caudal lobe is generally not processed for the time being (it may be necessary to process the donor liver in living donor liver transplantation). If you want to deal with it, you can use 5-0 sutures to ligate the proximal end of the blood vessel, and the distal computer feedback to control the bipolar electric knife (ligasure) or ultrasonic knife cutting.
The right hepatic artery is generally located between the right bile duct and the portal vein. It separates the bile duct and portal vein. After the portal vein is fully free, it is not difficult to look forward. After the right hepatic artery is free, the proximal upper vascular clip is clamped, and the distal end is cut directly with an ultrasonic knife or Ligasure. The reason why the vascular clip is not attached to the distal end is to avoid the impact of the vascular clip during the process of cutting off the right hepatic pedicle by the closing device, which may cause the nail to burst.
(4) Mark the hepatic ischemia line and determine the plane of the broken liver: mark the ischemic line on the liver surface with an electrocoagulation hook. According to the ischemic line on the liver surface and the projection of the middle hepatic vein on the liver surface judged by laparoscopic ultrasound, the ischemia is determined The angle of the plane after the line is broken, or select a proper deviation from the right side of the ischemic line to cut the liver to ensure that the middle hepatic vein is preserved.
(5) Treatment of the short hepatic vein: The treatment of the short hepatic vein follows the principle from the foot side to the head side. When encountering a short hepatic blood vessel, first cut it out with a right-angle forceps, then tie a knot with a sling, and use a hemo-lock clamp on the side of the vena cava. For clipping, the liver side can be clipped with a heme-lock clip or a titanium clip and then cut off, or it can be cut off directly by Ligasure. Larger short blood vessels in the liver can also be cut off with a closure device. After the short hepatic vein is processed, the right vena cava ligament is disconnected.
(6) Double main knife + CUSA to cut the liver parenchyma: The surgeon on the right uses an ultrasonic knife with his right hand to split the liver parenchyma along the liver surface, then switches to CUSA with his right hand, and pulls the liver with the separation forceps in the left hand. The surgeon on the left uses an ultrasonic knife with his left hand, and his right hand holds the Beike forceps (bipolar electrocoagulation) or the low-temperature radiofrequency bipolar hemostatic system (AQM) to gradually cut off the liver parenchyma from shallow to deep.
CUSA can not only shatter the liver cells to leave the duct structure, but also play a part of the function of the suction device. When encountering the duct structure, the operator on the left side can replace the clamp with the hemo-lock clamp. Note that sometimes large pipes need to be completely exposed from the back with right-angle pliers or golden fingers. As the liver is severed, you will generally encounter the V and VIII branches of the middle hepatic vein. Pay attention to protect it to avoid tearing or accidental interruption of the ultrasound knife and cause hemorrhage.
The hepatic parenchyma needs to reach the hilar plate structure around the bile duct of the first hepatic hilar. At this time, the liver parenchyma is split from the center of the caudate lobe in front of the inferior vena cava. This process should be close to the dorsal side of the right liver pedicle, from the foot side to the head side.
(7) Disconnect the first hepatic portal on the right side: Use a cutting closer to disconnect the first hepatic portal on the right side. This step must be marked with the clip or ligature on the right branch of the portal vein to avoid being too close to the left side to cut off, resulting in stenosis of the left bile duct after surgery.
(8) Disconnect the right hepatic vein: After disconnecting the duct structure of the first hepatic hilum on the right side, disconnect the remaining liver parenchyma to the cephalic side, and the right hepatic vein can be reached soon. If the sling has been preset behind the liver, the sling can be directly pulled forward to facilitate disconnection, and it can reach the right hepatic vein directly. Before handling the right hepatic vein, it is best to suspend it. If it is sufficiently freed, there is no problem if it is not suspended.
It is recommended to operate the right hepatic vein close to the inferior vena cava. Golden fingers and some special types of vascular clamps can be used to improve efficiency, and catheterization can also be used. After the right hepatic vein is fully freed, the right hepatic vein is disconnected using a cutting closure device.
(9) The excised specimens need to be put into a specimen bag of appropriate size and taken out: the specimens are usually taken out according to the size of the specimens by connecting the poke holes on the midline in longitudinal rows and cutting them. It can be extended appropriately according to the different distance between the two poke holes, generally between the two poke holes, or you can consider making another transverse incision on the pubic symphysis to take out the specimen.
(10) Treatment of liver section, fixation of residual liver, and placement of drainage tube: Continuously suture the incision to take the specimen with the abdomen thread, keep the original poke hole with interrupted suture and place the thread without ligation, and place the poke card and surgical instruments again. Check the liver section for hemorrhage and gallbladder leakage, if necessary, suture with 4-0 prolene suture. Flush the abdominal cavity repeatedly, and after confirming that it is correct, hemostatic materials can be placed on the liver section. The falciform ligament stump was sutured again to fix the residual liver, and finally the liver section and Venturi foramen were placed for drainage, and the operation was completed.
4. Summary and analysis of surgical details
Intraoperative laparoscopic ultrasound applications include: judging whether the structure of the hepatic hilar duct is altered; verifying the correctness of the anatomy of the hepatic hilar; marking the projection of the middle hepatic vein on the liver surface; marking the planned resection line and adjusting the plane of the broken liver, etc. several aspects.
The team used the double main knife + CUSA method to optimize the method of liver parenchymal dissection, and gave full play to the advantages of two surgeons at the same time, avoiding the time waste caused by different surgical instruments repeatedly entering and leaving the abdominal cavity during the single main knife operation, and integrating various energies The advantages of the instrument improve the efficiency of liver severance and shorten the operation time. Moreover, this optimized method, through the rational use of CUSA, can achieve the engraving of the intrahepatic duct, effectively avoiding bleeding that is difficult to control during the hepatectomy.
The team used selective hemihepatic blood flow block + intermittent total hepatic blood flow blockade to control the first hepatic portal hepatic blood flow, and at the same time cooperated with controlled low central venous pressure to cut off the liver parenchyma process The bleeding was significantly reduced, and the surgical field remained clear. Thus, the remaining liver function is ensured, the operation time is shortened, and the safety of the operation is improved.
The second hepatic portal treatment is another key. The team recommends that the right hepatic vein should not be dissected out of the liver routinely. Instead, it is advisable to dissect the right hepatic vein in the liver and close it when approaching the second hepatic hilum in the later stage of the hepatic parenchyma. Because hepatic veins are easy to tear and cause uncontrollable bleeding, and after tearing, it is likely to cause air embolism, which can cause death in severe cases.
Of course, if the local tissue is loose and the level is clear, extrahepatic anatomy and suspension of the right hepatic vein can also be considered. This has certain advantages for the protection of blood vessels and the judgment of the plane of the liver when anatomically resected tumors in some special parts.
It is best to use a sling (line) when severing the right hepatic pedicle and right hepatic vein during the operation. After suspending the pipeline structure, insert the cutting closer, and be sure to see the end of the staple cartridge and the reserved side to avoid bleeding And pre-save the damage of the side pipeline. For patients with hepatolithiasis, before cutting the closure device to treat the right hepatic pedicle, it is necessary to determine the fracture plane through laparoscopic ultrasound to exclude intrahepatic bile duct stones, so as to avoid accidental nail bursts.
For the treatment of short hepatic blood vessels, it can be temporarily closed with a small titanium clip or hemo-lock clip. It is recommended to ligate the blood vessel with sutures after removing the specimen to increase reliability. Regarding the liberation of the ligaments around the liver, generally the right hepatectomy does not necessarily completely free the left hepatic ligament, but it is recommended that at least the left coronary ligament be freed to facilitate the rotation of the liver and facilitate exposure.
The choice of surgical approach should not be limited to a certain method. For patients with large tumors, difficult to move, and a history of interventional embolization or radiofrequency ablation, the relationship between the liver and the diaphragm or abdominal wall is often relatively dense, and it is quite difficult to free the liver. The author believes that in this case, the use of anterior approach to cut the liver or a combination of the two methods may be more conducive to the complete resection of the tumor, and avoid unnecessary tumor rupture, which may increase the risk of implantation and metastasis.
- Recommended news
- 【General Surgery Laparoscopy】Cholecystectomy
- Surgery Steps of Hysteroscopy for Intrauterine Adhesion
- [Thoracoscopic Surgery] Thoracoscopic Radical Resection of Lung Cancer
- [General Surgery Laparoscopy] 4K ultra-high definition laparoscopic hiatal hernia repair
- [General Surgery Laparoscopy] 4K Ultra HD Laparoscopic Surgery for Acute Cholecystitis