[Thoracoscopic surgery of thoracic surgery] 4K ultra-high definition thoracoscopy for esophageal leiomyoma
Release time: 16 Jan 2024 Author:Shrek
Esophageal leiomyoma is a benign tumor that grows on the esophageal wall. It originates from the muscular layer of the esophageal wall and grows slowly into and out of the lumen without invading the mucosa and submucosa. The tumors are small and usually have no obvious symptoms. As the tumor gradually increases, some patients may develop retrosternal discomfort, difficulty swallowing, and loss of appetite. After the esophageal leiomyoma is stretched, it will cause gastrointestinal bleeding, manifested as vomiting blood or vomiting brown liquid.
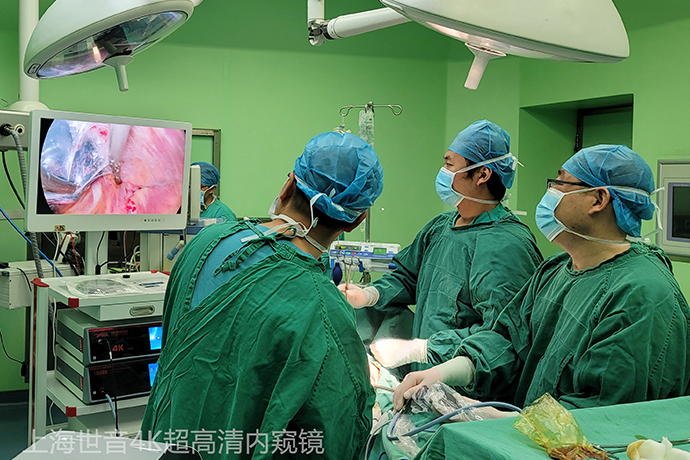
The probability of malignant transformation of esophageal leiomyoma is low, so patients do not need to worry too much. When the tumor is small and the patient is asymptomatic, surgery is not required and the changes in the condition can be observed. For patients with clinically symptomatic esophageal leiomyoma, the tumor can be removed through gastroscopy or surgery. Only through surgical resection can esophageal leiomyomas be completely cured.
Is minimally invasive surgery for esophageal leiomyoma dangerous?
I had not been eating regularly before, and I often felt bad about my stomach and digestion, so I got esophageal leiomyoma. The doctor said I needed tumor surgery and suggested minimally invasive surgery. I don’t know if it’s dangerous. Esophageal leiomyoma Is minimally invasive surgery effective?
Is minimally invasive surgery for esophageal leiomyoma dangerous? answer:
Esophageal leiomyomas are benign tumors that are generally located under the mucosa. There are no obvious symptoms of discomfort. During the physical examination, it is found that if the leiomyoma is relatively large, it can cause choking when eating. At present, surgical treatment is mainly adopted after diagnosis. Surgery can be performed through thoracoscopic esophageal leiomyoma removal, and cure can be achieved after surgery. It is recommended to visit the thoracic surgery department of a regular hospital for diagnosis and treatment.
More answers:
Esophageal leiomyomas are relatively common benign tumors that can cause different clinical symptoms such as vomiting, eating infarction, and dysphagia. Small esophageal leiomyomas can be observed, but if they increase significantly and cause the above symptoms, it is recommended to consider them in time. Minimally invasive surgery has less trauma and faster recovery after surgery, but any surgery has certain risks, and the doctor will inform you in detail before the surgery.
Esophageal leiomyoma is a rare benign lesion of the esophagus. Most of them have no obvious symptoms. Most of them originate from the muscle layer, and a few originate from the mucosal muscle layer. They are irregular in shape, such as round, horseshoe-shaped, etc., and are mostly solitary. In recent years, with the development of endoscopic technology, its treatment methods have gradually changed from surgery to endoscopic treatment. The main endoscopic resection methods include ESD and submucosal tunneling endoscopic resection (STER). Esophageal leiomyoma is a common benign tumor in the esophagus, accounting for approximately 70% to 80% of benign esophageal tumors. The esophageal wall is composed of mucosal layer, submucosal layer, muscular layer and adventitia. Esophageal leiomyomas, regardless of their location, shape and size, are generally located in the esophageal smooth muscle layer and do not invade the mucosal layer.
It is understood that tumors with a diameter less than 2 cm only require follow-up observation. Single or multiple leiomyomas in various parts of the thoracic esophagus with a tumor diameter ≥ 2 cm may have the following three situations:
1. If the tumor is round or oval, it is easiest to remove.
2. The tumor is spiral or other irregular shape, and the esophageal mucosa is easily damaged during surgery, so it must be completed through thoracoscopy and a small incision.
3. The muscle layer of giant esophageal leiomyoma is atrophied, thin or damaged. After the tumor is removed, the damaged muscle layer is too large to be repaired, and esophagectomy is often required.
Note: If esophageal leiomyoma is found under endoscopic ultrasound, do not perform a biopsy to avoid damaging the mucosa. Intraoperative gastroscopy was performed to determine whether there was any esophageal mucosal damage. In order to completely remove the tumor and preserve the functionality of the esophagus and azygous arch, minimally invasive but difficult thoracoscopic surgery is performed.
Because the structure of the submucosa at the junction of the lower esophagus and the fundus of the stomach is different, we should be alert to the occurrence of infection, perforation, and esophageal fistula after surgery. This patient's body temperature increased and subcutaneous emphysema occurred after surgery, which was caused by the large surgical wound. After anti-infection and fluid rehydration support treatment, the body temperature recovered and the subcutaneous emphysema was reduced. Subsequent gastroscopy showed no obvious fistula. Therefore, it is still recommended to perform ESD resection for esophageal leiomyomas with larger lesions, combined with thoracoscopic or laparoscopic resection when necessary. At the same time, higher requirements are placed on the operating physician. They must be careful to prevent perforation while completely resecting the lesion, and pay close attention to the patient after surgery. Changes in condition.
Warm reminder: Esophageal leiomyoma is the most common benign esophageal tumor, which can occur in all ages, with a high incidence in those aged 20 to 50 years. Many people are careless when they see benign tumors; however, esophageal leiomyomas need to be treated early, otherwise the condition will continue to worsen and eventually become life-threatening. If you have difficulty swallowing, pain and discomfort and other digestive tract symptoms in your daily life, you should pay attention to it, come to the hospital as soon as possible and actively and formally handle it in the early stage.
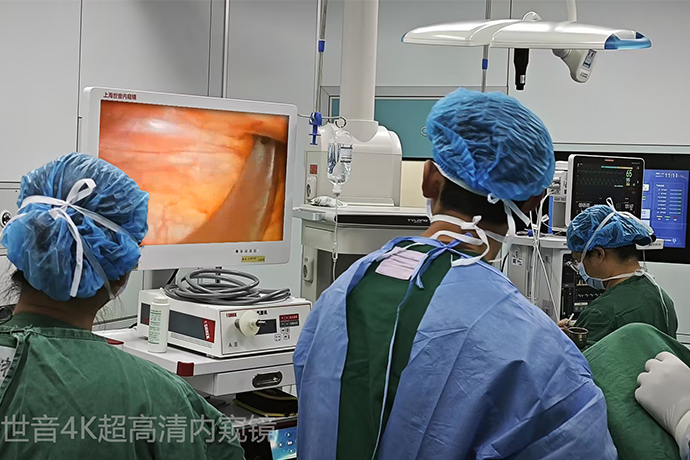
- Recommended news
- 【General Surgery Laparoscopy】Cholecystectomy
- Surgery Steps of Hysteroscopy for Intrauterine Adhesion
- [General Surgery Laparoscopy] 4K Ultra HD Laparoscopic Surgery for Acute Cholecystitis
- [General Surgery Laparoscopy] 4K ultra-high definition laparoscopic deroofing and decompression of renal cysts
- [Ureteroscopy in Urology] Laser lithotripsy for ureteral stones