【Gynecological Hysteroscopy】Hysteroscopic hysterectomy
Release time: 30 Aug 2022 Author:Shrek
In the treatment of infertility, some patients are often required to go for hysteroscopy and treatment for various reasons.
Although hysteroscopic surgery is a small operation, some patients are often very nervous about it. The most frequently asked question is: "Doctor, why should I do hysteroscopic surgery? Is it painful? Can I not do it? Can't conservative treatment work?"
Some people liken the mother's uterus to the cradle of the baby's sleep, while others liken the endometrium to the land where the seeds germinate. Before we put the baby in the cradle, we usually need to lay out a quilt to check whether the quilt is thick enough and whether there are other things in the cradle that should not be there.
Before planting seeds in the soil, we also need to weed, turn the soil, sprinkle some water, and fertilize. The same is true for the preparation of the uterus before transplantation. In addition to fertilizing and watering, other things such as checking the bed, turning the soil and weeding, etc., have to be done by another technique, that is, hysteroscopy.
What is a hysteroscopy?
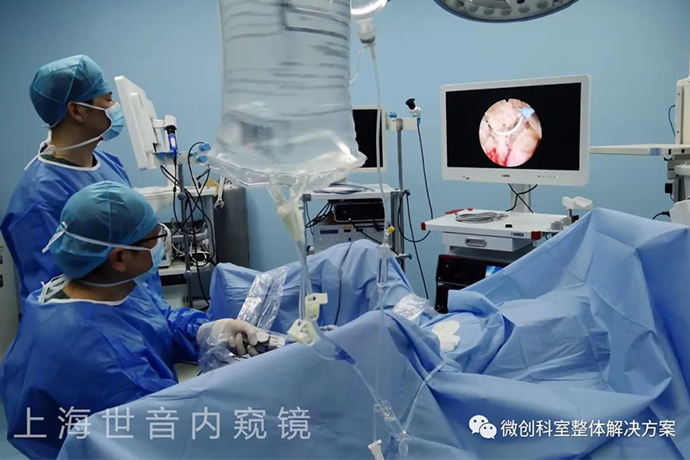
Hysteroscopy is a light source endoscope that can be used for the diagnosis of causes of infertility, and the diagnosis, treatment and follow-up of lesions in the uterine cavity. Hysteroscopy can not only determine the location, size, appearance and scope of the lesion, but also make a detailed observation of the tissue structure on the surface of the lesion. The accuracy of disease diagnosis, update, development and make up for the shortcomings of traditional diagnosis and treatment methods.
Hysteroscopic surgery, as a minimally invasive surgery, can generally be done in an outpatient clinic. The whole process is intravenous anesthesia, and the patient is unconscious. It lasts about 10-30 minutes, and the degree of difficulty varies greatly and the time required varies greatly. Hysteroscopy is indicated for those suspected of having any form of intrauterine disease who need to be diagnosed and treated.
When do you need a hysteroscopy
1. Abnormal uterine cavity
It is a common gynecological disease. Polyps are caused by local hyperplasia of the endometrium, which manifests as single or multiple smooth masses protruding from the uterine cavity, which can cause irregular vaginal bleeding and infertility. B-ultrasound may suggest "endometrial polyps, uneven endometrial echo, endometrial thickening" and so on. Before doing IVF, if you find endometrial hyperplasia or polyps, you need to have a hysteroscopy first, so as not to affect the embryo implantation.
The incidence of endometrial polyps in infertile patients is 14.9% to 26.5%. Traditional ultrasonography, small endometrial polyps can be missed, while hysteroscopy can be diagnosed under direct vision, and it can be identified and evaluated. , treatment and biopsy.
2. Intrauterine adhesions:
Intrauterine adhesions will reduce the embryo implantation rate, especially severe intrauterine adhesions. Therefore, hysteroscopic separation of the uterine adhesions is required before embryo transfer to open the uterine cavity with adhesions. For mild adhesions, use an alternative cycle of 1-3 months after surgery; for moderate or severe adhesions, an IUD may be placed after surgery to avoid re-adhesion, and hysteroscopic surgery will be performed again to remove the IUD, or after surgery An intrauterine balloon was then placed and removed one week after surgery. It is worth noting that severe intrauterine adhesions may require multiple surgeries.
For some infertile patients, hysteroscopic surgery can also observe the anatomical shape of the opening of the fallopian tube and the fluid flow of the fallopian tube intubation to determine the degree of patency.
Surgical steps of hysteroscopic resection of intrauterine adhesions
(1) Fill the bladder, carefully place the probe under the guidance of B-mode ultrasound, and dilate the cervix and uterine cavity one by one with dilation. In the case of uterine atresia, when the probe cannot reach the fundus of the uterus or only probes into the cervical canal, it can be opened later by hysteroscopic surgery, or the probe can be pushed forward along the cervix and uterine midline under the supervision of B-mode ultrasound. Palace bottom
(2) Under the guidance of B ultrasound, the hysteroscope was inserted into the uterine cavity along the external cervical os and cervical canal. Check the shape of the cervical canal and the uterine cavity, observe the bilateral uterine angle and the opening of the fallopian tube, reveal the adhesion tissue, and determine the location and degree of the adhesion.
Under the guidance of B ultrasound, the hysteroscope was inserted into the uterine cavity along the external cervical os and cervical canal. Check the shape of the cervical canal and uterine cavity, observe the bilateral uterine angle and the opening of the fallopian tubes, reveal the adhesion tissue, and determine the location and degree of adhesion.
(3) The dense adhesion scar tissue in the cervical canal can be removed with needle electrode of hysteroscopic resectoscope or ring electrode.
(4) The central membranous or fibrous adhesion tissue in the uterine cavity can be cut by hysteroscopic needle electrode or ring electrode resection. The normal endometrium needs to be protected during surgery.
(5) For the adhesion scar tissue on the anterior, posterior and lateral walls of the uterine cavity, needle electrodes can be used to cut along the long axis of the uterus, and if necessary, ring electrodes can be used for electrical resection.
(6) The adhesion of the uterine fundus and the uterine horns needs to be cut horizontally with needle electrodes or horizontally cut with ring electrodes to completely open the fundus. At the same time, the incision moves to the uterine horns, and the bilateral uterine horns are opened as much as possible to expose the opening of the fallopian tubes. Generally, under the supervision of B-mode ultrasound, needle electrodes are used to separate the adhesions at the male corners, and if necessary, ring electrodes are used to cut the adhesion tissue, gradually reveal the uterine horns and the opening of the fallopian tubes, and restore the normal shape of the bilateral uterine horns. Care should be taken to protect the normal endometrial tissue at the uterine angle.
(7) For uterine cavity constriction caused by uterine wall scar spasm, needle electrodes can be used to cut 4-5 scar tissue longitudinally and radially along the long axis of the uterus to expand the uterine cavity volume.
(8) If the uterine cavity is closed and there is a blind end in front of the scope, under the supervision of B-mode ultrasound, the needle electrode or ring electrode can be energized and gently pushed forward along the midline of the cervix and uterus to try to open the adhesion tissue and cut out Pores, revealing the uterine cavity. Then follow the above steps to remove the intrauterine adhesions and restore the normal uterine cavity shape.
(9) At the end of the operation, the objective lens was withdrawn to the internal os of the cervix to observe the shape and symmetry of the uterine cavity.
(10) At the end of the operation, retract the objective lens to the internal os of the cervix to observe the shape and symmetry of the uterine cavity.
Hysteroscopic scissors separation of intrauterine adhesions
(1) Perform hysteroscopy first. A hysteroscope was placed, and the shape of the uterine cavity and the condition of intrauterine adhesions were examined under direct vision.
(2) The flexible semi-rigid scissors or rigid scissors are delivered to the uterine cavity along the operation channel of the hysteroscope.
(3) Use hysteroscopic scissors to gradually separate the adhesions from the center of the uterine cavity to the surrounding areas to expand the uterine cavity. If the adhesion is extensive, attention should be paid to the depth of the separation of the adhesion, and be alert to the occurrence of uterine perforation. When separated to the bus, the uterine horn should be freed as much as possible under the guidance of B-mode ultrasound to expose the opening of the fallopian tubes.
When the uterine cavity or cervical canal is completely closed, it should start from below the adhesion, and gradually separate along the midline of the uterus under the guidance of B-mode ultrasound until a new uterine cavity is opened.
Cervical abnormalities
1. Cervical polyps: If cervical polyps are found before IVF, hysteroscopy is recommended first, because polyps may block the cervix and cause difficulty in embryo transfer or bleeding, and it is difficult to distinguish polyp bleeding from intrauterine bleeding after pregnancy.
2. Cervical adhesions: Injury to the cervix from the uterine cavity operation may cause cervical adhesions and make embryo transfer difficult. This also requires hysteroscopy to separate adhesions.
Gynecological related diseases
Some diseases related to gynecology require hysteroscopy such as
1.Abnormal uterine bleeding: such as menorrhagia, excessive frequency, prolonged menstruation, and irregular vaginal bleeding, hysteroscopy should be performed after excluding pregnancy.
2. After hormone replacement therapy or oligomenorrhea: Long-term use of hormone therapy or oligomenorrhea (such as polycystic ovary syndrome) may cause endometrial hyperplasia, polyp formation, and endometrial cancer in severe cases. Hysteroscopy and evaluation are required.
Unexplained infertility, habitual abortion
Hysteroscopy is recommended to exclude abnormalities that cannot be detected by imaging examinations.
Hydrosalpinx
Hydrosalpinx is one of the important factors affecting embryo implantation. The traditional surgical method is to remove or ligate the fallopian tubes through laparoscopic surgery, which requires hospitalization and surgery under general anesthesia. Hysteroscopic tubal embolization is to place a microcoil into the interstitial part of the fallopian tube under the direct vision of a hysteroscope, thereby preventing the backflow of fluid into the uterine cavity.
The advantages are that the process is short (about 10-20 minutes), the operation is simple, and the cost is lower than that of laparoscopy, but it takes 2-3 months after the operation to perform IVF treatment.
Other rare cases
If a diverticulum is formed at the cesarean section, making it difficult to transplant, hysteroscopy is required to clarify the location and depth of the diverticulum to guide the next embryo transfer.
Repeated embryo implantation failure
Repeated implantation failure refers to those who failed to transfer ≥3 high-quality embryos or failed to transfer a total of ≥10 embryos. Although B-ultrasound may indicate no obvious abnormality of the endometrium, hysteroscopy is also recommended to exclude endometrial problems that are difficult to detect by B-ultrasound, such as mild intrauterine adhesions.
Even if the hysteroscopy shows no abnormalities, mild scratching can stimulate the endometrium and improve the endometrium environment, possibly making implantation easier after the next embryo transfer.
Hysteroscopic surgery time and precautions
Hysteroscopic surgery can be carried out after menstruation is clean. For example, it is better to perform tubal drainage no later than 5 days after cleaning. Otherwise, the endometrium will be too thick and the uterus will be prone to edema, which will affect the surgical field of vision.
Depending on the condition of the endometrium in different patients, the doctor in charge decides to perform surgery in each period of the menstrual cycle.
Intercourse is prohibited 3 days before surgery.
Before surgery, avoid eating greasy food and being too full, and drink less water.
The operation takes about ten minutes to half an hour, and you can leave the hospital after resting and observing for half an hour.
Family members are required to accompany you if anesthesia is required.
There is no need to stay in bed after the operation, but you should not be tired. Intercourse is forbidden for two weeks after the operation.
Normal diet, avoid spicy, blood-activating food.
If an intrauterine device (upper ring) is placed, it is normal to experience backache, falling, and bleeding, and no need to seek medical attention. Severe abdominal pain and continuous heavy bleeding came to the center for examination. You can resume your previous fitness activities without discomfort.
After the second menstrual period of the patient with the IUD (upper ring) is clean, the ring is taken from the center. If it is difficult to completely clean, there is no blood and only brown secretions will not affect the operation.
NO1. Uterine perforation
(1) Reasons: High-risk factors for uterine perforation include cervical stenosis, history of cervical surgery, excessive uterine flexion, small uterine cavity, and inexperienced operators.
(2) Clinical manifestations: ①The uterine cavity is collapsed and the vision is unclear. ② Ultrasound showed that free fluid around the uterus or a large amount of perfusate entered the abdominal cavity. ③ The peritoneum, bowel or omentum can be seen in hysteroscopy. ④If there is laparoscopic monitoring, the uterine serous surface is clear, blisters, bleeding, hematoma or perforated wounds. ⑤The electrode enters and damages the pelvis and abdominal organs, causing corresponding complications and symptoms.
(3) Treatment: ① First, find the perforation site, determine whether the adjacent organs are damaged or not, and decide the treatment plan. ②When there is no active bleeding and organ damage, oxytocin and antibiotics can be used, and observation can be made. ③When the perforation is large in scope and may damage blood vessels or organs, laparoscopic or laparotomy should be performed immediately and corresponding treatment should be carried out.
(4) Prevention: ①Strengthen cervical pretreatment and avoid violent uterine expansion. ② Combined ultrasound or laparoscopic surgery as appropriate. ③Improve the surgeon's surgical skills. ④Use GnRH-a drugs as appropriate to reduce the volume of fibroids or uterus, and to thin the endometrium.
NO2. Bleeding
(1) The main reason: the destruction of the myometrium below the endometrium is too deep.
(2) Risk factors for bleeding include: uterine perforation, arteriovenous fistula, placenta accreta, cervical pregnancy, cesarean section scar pregnancy, and coagulation dysfunction.
(3) Treatment: ① Generally, the bleeding point of the cervix is not easy to stop the bleeding. Because of the poor contraction of the cervix, the bleeding of the cervix can be packed with gauze soaked with vasopressin diluent (30ml normal saline + 20U vasopressin). Stimulates uterine contractions and is removed 8-12 hours after surgery. ②The blood vessels in the deep myometrium are incised. When electrocoagulation is difficult to stop bleeding, a Foley catheter can be placed. The volume of the normal uterine cavity is 5-10ml, and 15-30ml can be injected for severe bleeding in the larger uterus. Patients with uterine fibroids need 30-60ml. Because the balloon is in close contact with the uterine wall after being inflated, the uterine wall is evenly stressed, and it can be compressed to stop bleeding, which is multi-functional. Generally, the balloon can be placed for 12-24h to fully stop the bleeding. Note that antibiotics should also be given to prevent infection.
(4) Prevention: ①Try to make the endometrium thinner to facilitate excision, such as preoperative drug treatment or intraoperative curettage and then endometrial excision. ②Ensure that the perfusate has sufficient flow rate to keep the surgical field clear. ③The depth of endometrial resection should be 2-3mm below the endometrium. Because the vascular layer of the uterine muscle wall is located 5-6mm below the endometrium, if the excision is too deep, the damage to the vascular layer can cause massive bleeding, which is difficult to control. ④The excision wound should be smooth and flat, which is helpful to see the blood-spraying blood vessels clearly. Blind electrocoagulation is often not ideal for bleeding points hidden behind or between tissues that are difficult to see, and the raised tissue should be excised to reveal the bleeding point before hemostasis can be successful. ⑤Sequential cutting, each cutting a site until hemostasis is complete, and then cut the next site. Avoid large wounds and excessive bleeding. Multiple bleeding can easily lead to blurred surgical field and affect the operation.
NO3. Gas embolism
(1) Reason: tissue gasification and indoor air during the surgical operation may enter the venous circulation through the open blood vessels of the uterine cavity, resulting in gas embolism.
(2) Clinical manifestations: The onset of gas embolism is sudden, the progress is rapid, the early symptoms such as end-expiratory PCO2 drop, bradycardia, PO2 drop, the precordial area hears a large water wheel sound, etc.: followed by increased blood flow resistance, cardiac output The amount decreased, cyanosis, hypotension, shortness of breath, cardiopulmonary failure and death occurred.
(3) Treatment: stop the operation immediately, inhale oxygen at positive pressure, and correct cardiopulmonary failure. At the same time, normal saline was injected to promote blood circulation, central venous catheter was placed, and cardiopulmonary arterial pressure was monitored.
(4) Prevention: ①Avoid the posture with the head low and the hip high. ②Evacuate the gas in the water injection pipe before the operation. ③Carry out cervical pretreatment to avoid cervical laceration caused by rough dilation of the uterus. ④Strengthen intraoperative monitoring and emergency treatment.
NO4. Perfusate overabsorption syndrome
(1) Reasons: The pressure of uterine distention and the use of non-electrolyte perfusion media during hysteroscopic surgery can allow liquid media to enter the patient’s body. When the absorption threshold is exceeded, it can cause fluid overload and dilutional hyponatremia, and cause cardiac Corresponding changes in important organs such as brain, lung, etc., appear a series of clinical symptoms.
(2) Clinical manifestations: including increased or decreased blood pressure, slow heart rate, nausea, vomiting, headache, blurred vision, restlessness, mental disorder and lethargy, etc. If the diagnosis and treatment are not timely, convulsions, cardiopulmonary failure and even death will occur.
(3) Predisposing factors: intrauterine high pressure, massive absorption of perfusion media, etc.
(4)Treatment: ①Oxygen inhalation, diuresis, treatment of hyponatremia, correction of electrolyte imbalance and water intoxication. ②treatment of acute left heart failure, prevention and treatment of pulmonary and cerebral edema. ③Special attention should be paid to the correction of dilutional hyponatremia, which should be calculated and supplemented according to the formula of sodium supplementation: required sodium supplementation = (normal serum sodium value - measured serum sodium value) 52% X body weight (kg). ④The hysteroscopic bipolar electrical system uses normal saline as the intrauterine perfusion medium, which reduces the risk of hyponatremia, but there is still the risk of fluid overload.
(5)Prevention: ①Pretreatment of cervix and endometrium helps to reduce the absorption of perfusate. ②Keep intrauterine pressure ≤100mmHg or <mean arterial pressure. ③Control the difference of perfusate between 1000-2000ml. ④Avoid deep damage to the uterine muscle wall.
NO5. Preventive measures for intrauterine adhesions:
① Use needle electrodes to cut the mucosa and the capsule of the fibroids on the surface of the protruding fibroids in the uterine cavity, and then use the ring electrodes to cut the tumor body, try not to damage the normal endometrium around the tumor body to prevent secondary postoperative complications The key to sexual intrauterine adhesions. ②If there is a large exposed wound in the uterus or the preoperative application of GnRH-a treatment causes low estrogen in the patient's body, an appropriate amount of estrogen after surgery can stimulate the growth of the endometrium, accelerate the epithelialization process, and prevent the occurrence of intrauterine adhesions. ③IUD can also be placed during the operation. If there is a lot of bleeding during the operation, it can be placed after the menstrual cramps after the operation to prevent the occurrence of intrauterine adhesions with the help of the physical support of the IUD.
NO6. Infection
Strictly grasp the indications for surgery, surgery is contraindicated in the acute stage of genital tract infection, and antibiotics are used as appropriate to prevent infection after surgery.
- Recommended news
- 【General Surgery Laparoscopy】Cholecystectomy
- Surgery Steps of Hysteroscopy for Intrauterine Adhesion
- [General Surgery Laparoscopy] 4K ultra-high definition laparoscopic hiatal hernia repair
- [General Surgery Laparoscopy] 4K Ultra HD Laparoscopic Surgery for Acute Cholecystitis
- [General Surgery Laparoscopy] 4K ultra-high definition laparoscopic deroofing and decompression of renal cysts